Registered dietitian, functional nutritionist, & your new fertility BFF. I'm passionate about helping women thrive during preconception, pregnancy, and postpartum.
Nutrition
PCOS
Fertility
View All
Explore the blog
Hi, I'm Anabelle
Non-toxic Living
Work with our team
Why Fertility Awareness Matters (Whether or Not You are Trying to Conceive)
By: Josie Mangano
Reviewed By: Anabelle Clebaner MS, RDN
It’s commonplace for women to are trying to conceive to track their menstrual phases. However,
did you know that whether or not you’re trying to conceive, tracking the phases of your
menstrual cycle can be a valuable tool for assessing overall health and wellbeing? If you have
PCOS or are experiencing symptoms related to hormone imbalance, fertility awareness may
help you understand the cues your body is giving you in order to address the root causes.
Irregular menstrual cycles are linked to nutritional deficiencies, energy deficits, hormonal acne,
and even loss of bone density in the long-term. Put simply, your hormone health is important
even before you are trying to conceive.

What is Fertility Awareness?
Fertility awareness — is a set of practices that are used to determine the fertile and infertile
phases of your menstrual cycle.
The techniques used to track menstruation and ovulation are known as Fertility Awareness
Methods (FAMs). But first, let’s review what you should know about the menstrual cycle, the
fertile window, and what the patterns of a normal cycle look like.
What You Need to Know About the Menstrual Cycle
A normal menstrual cycle lasts anywhere between 24-35 days. The first day of your period
(when flow begins) is always considered day 1 of your cycle. Normal menstruation lasts
between 3-7 days.
In the days following menstruation, your ovaries release an egg into the fallopian tubes — this
process is called ovulation. This egg stays in your fallopian tubes and, if not fertilized by a
sperm, will dissolve after 12-24 hours. Contrary to the myth that ovulation occurs 14 days after
your period starts, ovulation typically happens between days 10-23, depending on the length of
your cycle. It is essential to note that sperm can survive in the female reproductive tract for up to
5 days. Therefore, your fertile window is classified as the 5 days before ovulation, the day of
ovulation, and the following day (7 days total).
During the fertile window, the sperm present in the female reproductive tract may fertilize an egg
and implant itself in the uterine lining, thus marking the beginning of pregnancy. If the egg is not
fertilized and the egg is reabsorbed, hormones drop, and menstruation occurs, marking the
beginning of a new cycle. After the fertile window passes, pregnancy is not possible because
the egg is no longer present for fertilization. The days after ovulation and before menstruation
are referred to as the post-ovulatory phase.
With that covered, we can dive into the science-backed tools we use for fertility awareness cycle
tracking.

The 3 main fertile signs to pay attention to are:
1. Cervical mucus
2. Basal body temperature (BBT)
3. Cervical position
Let’s review each of these signs more closely and learn how they may be related to underlying
causes such as hormone imbalances, nutrient deficiencies, and/or underlying health conditions.
Cervical Mucus
The presence of cervical mucus (CM) is indicative of your fertile window. CM plays an essential
role in natural conception by matching the pH of sperm, creating the perfect environment for it to
stay alive for up to 5 days in the otherwise hostile female reproductive tract.
There are two kinds of cervical mucus that are often referred to when it comes to reproductive
health. The first is “peak mucus” which is an optimal environment for sperm and is also an
indicator of a healthy cycle when present in the fertile window. Peak mucus is clear, stretchy,
and is comparable to egg whites. There is also “non-peak mucus” which is cloudy, white, and similar to creamy hand lotion. Non-peak mucus is not as optimal because it is hostile to sperm.
It is usually present shortly after menstruation and later in the menstrual cycle (luteal phase).
However, it is important to note that all mucus is fertile in the pre-ovulatory phase! Pregnancy
can occur in the presence of either kinds of CM in the fertile window

If your experience with CM differs, there are some red flags we can look for to assess
underlying hormonal imbalances and/or health conditions.
Cervical Mucus Red Flags
Limited or no mucus — can indicate an issue with hormone production, the cervix, or other
related issues including HPV, cervical dysplasia, or use of medications like hormonal birth
control, fertility drugs, or antihistamines. Can indicate inadequate nutrient intake of cholesterol
(to support estrogen and progesterone production), vitamin A, and B vitamins (folate). Can
indicate endocrine issues such as thyroid disorder, HPA axis dysregulation, hypothalamic
amenorrhea, etc.
Continuous mucus — can indicate an issue in the cervix, or presence of infection,
inflammation, or hormone imbalance.
Continuous creamy/lotiony (non-peak) mucus — may indicate an overgrowth of
yeast/bacteria. During the luteal phase, low progesterone production may contribute to
continuous non-peak mucus.
Continuous clear/stretchy (peak) mucus — seen in women with PCOS and/or women
experiencing food sensitivities, IBS, and other gut-related issues in the pre-ovulatory phase.
Yellow-tinged mucus – can be indicative of infection.
Basal Body Temperature (BBT)
Basal Body Temperature can be measured by taking your temperature first thing in the morning,
before getting. It is important that you do this immediately after waking up for an accurate
reading, before eating or drinking.
Tracking these temperatures provides us with the information we need to confirm when
ovulation occurs, but keep in mind that there is no way to predict when ovulation will occur due
to extraneous factors like travel and stress which may delay ovulation. You can keep track of
your BBTs by either logging them manually on a BBT chart or by using a fertility tracking app.
Normal pre-ovulatory temperatures should consistently be above 97.5° F ranging up to about
98.2 °F. Normal post-ovulatory temperatures should be higher than the pre-ovulatory range with
at least one temperature higher than 98.6 °F. Temperatures that fall consistently lower than this
range indicate potential health issues and nutrient deficiencies.

What are Some Possible Causes of Low Basal Body Temperatures?
Possible causes of low BBT include nutrient deficiencies of nutrients involved in thyroid function
such as zinc, iron, selenium, and iodine. Iron deficiency may also contribute to low BBTs since
iron is highly involved in body temperature regulation. Zinc and iron supplementation have
independently been shown to improve thyroid hormone levels and thus increase BBTs in
deficient women.
Low BBTs may also result from inadequate calorie consumption from skipping meals or failing
to consume enough calories to offset exercise levels. Poor sleep may also contribute to low
BBTs by offsetting natural circadian rhythms. Finally, thyroid disorders such as hypothyroidism
and Hashimoto’s thyroiditis play a role in lowering BBTs.
Cervical Position
The final indicator of fertility is cervical position, which changes throughout the menstrual cycle.
By regularly checking cervical position we can better understand our bodies through common
patterns that we notice throughout our cycles.
But what is the cervix and how can we use it to track our cycles?
The cervix is the small, muscular organ that connects the vagina to the uterus. It’s a round,
prominent structure with a hole in the middle that’s roughly an inch in diameter. It produces
cervical mucus, expels menstrual flow, allows sperm to pass through during ovulation, and acts
as a barrier against infections.
During ovulation, high estrogen levels cause the cervix to rise closer to the top of the vagina.
The cervix often feels softer during the fertile window. As mentioned previously, the cervix is
responsible for producing peak CM during this time.
After ovulation (luteal phase), the position of the cervix lowers to prepare for menstruation. This
cervix tends to lower or “drop” on average a week to 10 days before menstruation begins.
During menstruation, the cervix remains low and opens slightly to release the menstrual blood
flow. The cervix feels firm to the touch during this time and will continue to feel this way until
after your period ends.
In early pregnancy, the position of this cervix is high in the vagina, similar to its position during
ovulation. The cervix is known to feel soft during this time, however it is important to use a
pregnancy test to confirm pregnancy as cervical position is not a guarantee in confirming early
pregnancy.
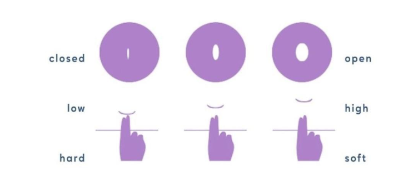
For more information on how to check your cervical position, click here.
Now that we’ve laid the groundwork of cycle tracking, let’s discuss some specific nutrients and
how they uniquely benefit cervical health!
Key Nutrients to Support Cervical Health
1. Folate — has been shown to reverse abnormal (precancerous) cervical cells and reverse
cervical dysplasia. Folate plays a key role in supporting healthy cell division, most notably
during early pregnancy in the formation of the spinal cord.
2. Vitamin A (retinol) — has been shown to reverse abnormal cervical cells when applied
topically to the cervix. Vitamin A is critical for fertility and plays a role in preparing the uterine
lining for implantation. Pregnant women should avoid all forms of vitamin A supplementation.
Dark leafy greens, red/orange vegetables, beef, eggs, and dairy products are rich in vitamin A.
3. Indole-3-Carbinol – has been shown to reverse abnormal cervical cells in clinical trials.
I3C plays a role in modulating estrogen metabolism and is a compound found in cruciferous
vegetables like broccoli, brussels sprouts, kale, and cauliflower

There you have it — the 3 main fertile signs to pay attention to and related cues that can give us
powerful insights into our hormonal and reproductive health. If you feel passionate about using
fertility awareness as a guide to managing hormonal imbalances, managing PCOS, or preparing
your body for the healthiest pregnancy possible, consider reaching out to our team at Wellspring
Nutrition for 1:1 functional nutrition counseling and a personalized plan to achieve your unique
health goals.
References
Hendrickson-Jack L. Women’s Health Nutrition Academy (WHNA). “Unlocking the Secrets of the
Menstrual Cycle: How Fertility Awareness Cycle Tracking Can Help Your Nutrition Practice”.
Sumner C. Cervix positions: What they mean & how to check them. Natural Cycles. Published
June 28, 2022. https://www.naturalcycles.com/cyclematters/cervix-positions-explained
Leave a Reply Cancel reply
The Preconception Playbook
This free playbook provides specific actionable tips to get started on your fertility journey, as well as what to avoid while you're trying to conceive.
Get the free playbook
Functional nutrition for women & couples trying to conceive
Get the Preconception Playbook
Actionable tips to get started on your fertility journey, as well as what to avoid while you're trying to conceive.
Be the first to comment