Nutrition
Resources
Style
Planning
View All
Menopause is often discussed in whispers and framed through negative stereotypes, yet it is one of the most significant and transformative stages of life. Understanding what’s happening in the body—and how to support it through nutrition and lifestyle—can help dismantle stigma and reframe menopause for what it truly is: a period of reflection, strength, and renewed autonomy.
To understand how functional nutrition supports menopause, it helps to briefly revisit how the menstrual cycle works before this transition. While this biology may feel basic, it provides essential context for understanding why symptoms arise and how targeted support can help.

Why Do Hormones Change So Much During Menopause?
Before menopause, the menstrual cycle is regulated by a tightly coordinated hormonal feedback system between the brain and ovaries.
The hypothalamus releases gonadotropin-releasing hormone (GnRH), which signals the pituitary gland to secrete luteinizing hormone (LH) and follicle-stimulating hormone (FSH). These hormones stimulate the ovaries to develop follicles, each containing an immature egg (ova).
As follicles mature, they release estrogen along with inhibin A and inhibin B. These hormones create a negative feedback loop, signaling the brain to slow the release of GnRH, LH, and FSH. After ovulation, the follicle becomes the corpus luteum, which produces progesterone to support the uterine lining. If pregnancy does not occur, progesterone levels fall and menstruation begins.
This predictable hormonal rhythm is what allows for regular cycles—and it’s this system that gradually shifts as menopause approaches.

What Happens to Hormones During Menopause?
Menopause typically begins around age 45, though timing varies widely and there is no “correct” age. Rather than a single event, menopause is a gradual process defined by the STRAW (Stages of Reproductive Aging Workshop) staging model.
Late Reproductive Stage (Stages −3A and −3B)
Cycles are usually regular, and pregnancy is still possible. However, ovarian reserve declines as fewer eggs remain available.
Early Menopause Transition (Stage −2)
This stage marks the beginning of perimenopause. Hormonal signaling from the brain increases, progesterone production becomes less consistent, and menstrual cycles often become unpredictable.
Late Menopause Transition (Stage −1)
Periods become very irregular, with gaps of 60 days or more between cycles. Hormonal fluctuations intensify, often leading to symptoms such as hot flashes, sleep disruption, mood changes, and weight gain. This phase can last up to three years, though duration varies.
Menopause (Stage 0)
Menopause is defined as the final menstrual period.
Early Postmenopause (Stages 1A and 1B)
These stages begin after 12 consecutive months without a period. Hormones continue to stabilize, but symptoms are often most pronounced during this time. Early postmenopause typically lasts two to six years as the endocrine system adjusts to a new baseline.
How Does Functional Nutrition Support Menopause?
Functional nutrition focuses on supporting the body’s changing hormonal, metabolic, and inflammatory needs during menopause rather than simply managing symptoms.
Nutrition for Hormone and Metabolic Health
A Mediterranean-style diet—rich in fruits, vegetables, whole grains, lean protein, and healthy fats—has been shown to reduce inflammation and support cardiovascular and metabolic health during menopause.
Soy-based foods may also help alleviate menopausal symptoms. Soy contains phytoestrogens, plant compounds that interact with estrogen receptors in the body. While phytoestrogens cannot replace estrogen, they can provide mild estrogen-like activity that may help ease symptoms associated with estrogen decline.
Flaxseeds are another valuable dietary tool. Rich in fiber, healthy fats, and lignans, flaxseeds have been shown to reduce the frequency and severity of hot flashes and night sweats. For best results, flaxseeds should be consumed consistently at approximately 2–3 tablespoons per day for at least 12 weeks.
Why Meal Timing Matters in Menopause
When we eat is just as important as what we eat. Late or irregular eating patterns are associated with weight gain and disruption of circadian rhythms that regulate sleep, stress hormones, and appetite. Consuming the majority of daily calories earlier in the day may support improved metabolic health, reduced inflammation, and more restorative sleep.
Movement and Nervous System Support
Regular physical activity—especially walking—has powerful benefits for both physical and mental health during menopause. Walking as little as 12.5 miles per week has been associated with reductions in anxiety and depression, along with improvements in sleep quality and insomnia symptoms.
Can Functional Nutrition Make Menopause Easier?
Menopause doesn’t have to be something you “just get through.” With the right nutritional and lifestyle support, it can be a time of empowerment, clarity, and renewed wellbeing.
Functional nutrition helps identify what your body needs during this transition—whether that’s blood sugar support, inflammation reduction, nutrient repletion, or nervous system regulation.
We’re Here to Support You
Navigating menopause can feel overwhelming, but you don’t have to do it alone. Our 1:1 coaching services provide personalized, functional nutrition support to help you feel informed, confident, and supported through every stage of menopause.
If you’re ready to invest in your health and wellbeing, we’d love to support you. Reach out today to begin your journey.
Sources:
Dr. Haylee Nye, Managing Menopausal Symptoms Naturally: Where to Begin (webinar)
Image Sources:
Organicauthority.com
Freepik.com

Why Routine Blood Work Matters for Women’s Health
Routine blood work is one of the most powerful ways to check in with your body and understand what’s really going on beneath the surface.
Your body can’t exactly tap you on the shoulder and say, “Hey, your vitamin D is low,” or “Your blood sugar is creeping up.” Instead, it communicates through subtle (and sometimes not-so-subtle) signs—fatigue, mood changes, stubborn weight, poor sleep, irregular cycles. While those symptoms are important clues, the most direct way to get answers is through routine blood work.
As a dietitian, I’m a big believer in using data to guide decisions—and I also believe it should be easy and accessible. That’s one of the reasons I personally decided to use Superpower for my own labs.
What Does “Routine Blood Work” Usually Include?
The term routine blood work is broad, but it typically includes several key tests that give a high-level snapshot of your health:
Complete Blood Count (CBC)
A CBC looks at red blood cells, white blood cells, hemoglobin, and platelets. These markers tell us how well your body is transporting oxygen, fighting infections, and clotting blood. Suboptimal levels can point to issues like anemia, inflammation, or underlying infections.
Comprehensive Metabolic Panel (CMP)
A CMP evaluates 14 different markers related to kidney function, liver function, electrolytes, blood sugar, proteins, and acid–base balance. This panel gives valuable insight into digestion, nutrient absorption, mineral status, and overall organ health.
Lipid Panel
This test measures LDL (“bad”) cholesterol, HDL (“good”) cholesterol, VLDL, and triglycerides. These markers reflect long-term dietary patterns, metabolic health, and cardiovascular risk. Elevated triglycerides or LDL can increase the risk of heart disease, while HDL plays a protective role by helping remove excess cholesterol from the bloodstream.
Thyroid Panel
A standard thyroid panel usually includes TSH, T4, and T3. These hormones regulate metabolism, energy, temperature, and growth. Imbalances here can show up as fatigue, weight changes, hair loss, or cycle irregularities—symptoms many women are told are “normal,” but often aren’t.
HbA1c
HbA1c reflects your average blood sugar over the past 2–3 months. It’s one of the most important markers for identifying insulin resistance, prediabetes, and diabetes.
- Below 5.7%: typical
- 5.7–6.4%: prediabetes
- 6.5% or higher: diabetes
My Personal Experience with Superpower
One of the biggest barriers I see—both personally and with clients—is logistics. Scheduling labs, remembering appointments, waiting weeks for results…it’s enough to make routine testing feel overwhelming.
That’s where Superpower really stood out to me.
The sign-up process was incredibly easy, and my blood work came back much faster than I expected. I also loved receiving text updates along the way—no guessing, no wondering when results would arrive.
Once I had my labs, the value really clicked. Having everything clearly laid out made it obvious where things were improving and where I needed support. I could see, for example, that my HbA1c had come down, which was incredibly validating, and that my vitamin D levels were lower than optimal, giving me clear direction on what to address next.
As someone who works with labs every day, I can confidently say: having this kind of insight makes it so much easier to make informed, proactive health decisions instead of guessing.
Making Blood Work Fit Into Your Life
If going to a doctor’s office or lab feels like one more thing on an already full to-do list, Superpower simplifies the process.
Superpower offers blood testing either at home or through one of their 2,000+ partner labs and assesses 100+ biomarkers—far more than what’s typically included in standard annual labs.
Beyond the testing itself, Superpower provides:
- A personalized plan based on your results
- Easy-to-understand data through their member portal
- Ongoing updates as your health evolves
- 24/7 chat access to their team if questions come up
Instead of just handing you numbers and sending you on your way, they help you understand what those numbers actually mean.
The Bottom Line
Routine blood work isn’t about finding something “wrong”—it’s about listening to your body before small imbalances turn into bigger issues. When testing is accessible, clear, and actionable, it becomes one of the most empowering tools for long-term health.
If you’ve been putting off labs because of time, logistics, or confusion around results, Superpower is absolutely worth checking out.
Learn more at: https://superpower.com
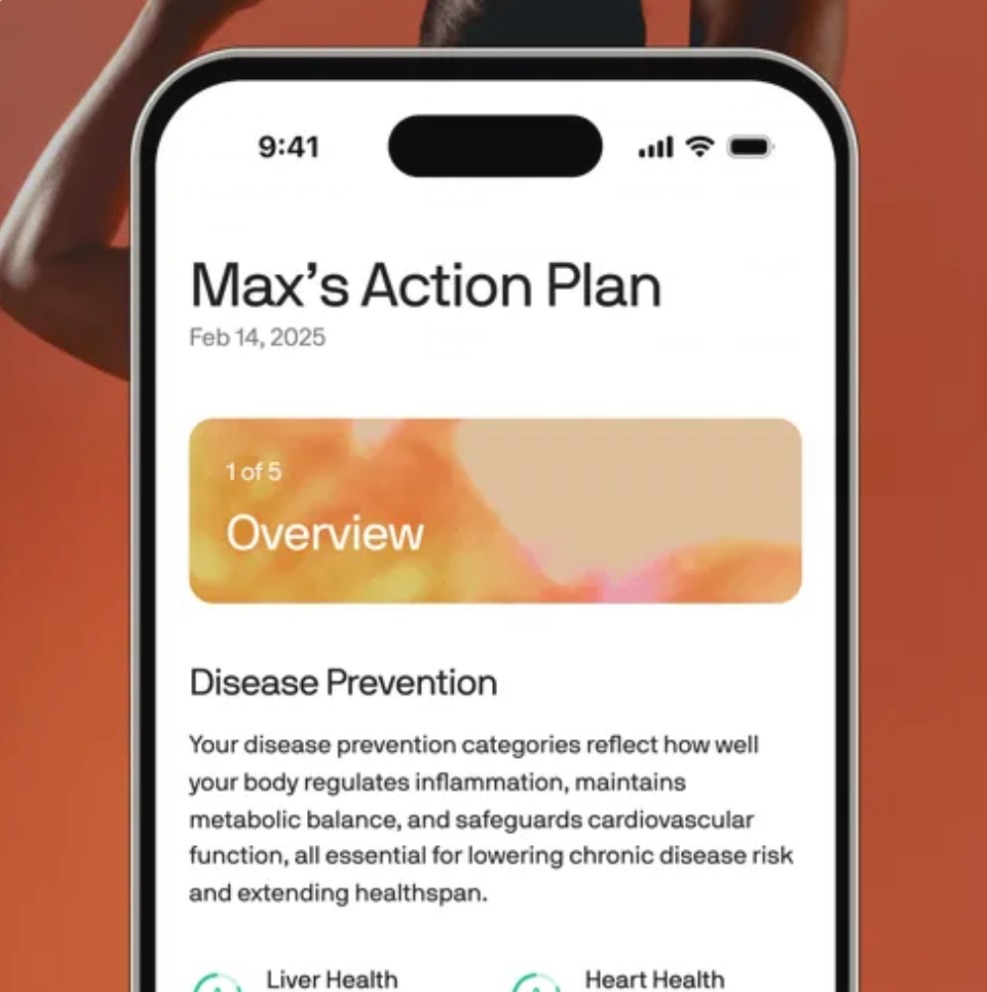
Superhero doesn’t stop there though, based on your bloodwork result a personalized plan is created that evolves with you. All of this data is easy for you to check and access through their website and member portal.

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Did you know that your gut health could impact more than just digestion? From immunity to mental clarity, a healthy gut plays a pivotal role in overall well-being—and even fertility. Emerging research suggests that a balanced gut microbiome influences hormone regulation, immune function, and inflammation, all of which are crucial for reproductive health. Whether you’re looking to optimize fertility or improve general health, supporting your gut can be a game-changer for both your body and mind.
The Basic Functions of the Gut
Before diving into the more intricate details of gut health, it’s essential to understand the basic functions of the gut and why it plays such a crucial role in your overall health.
1. Digestion
The gut is responsible for breaking down the food we eat, allowing nutrients to be absorbed into the bloodstream. This process starts in the mouth and continues through the stomach and small intestine. Enzymes and acids help break down food into smaller molecules for absorption.
2. Nutrient Absorption
Once food is broken down, the small intestine absorbs essential nutrients—like vitamins, minerals, and amino acids—into the bloodstream. These nutrients are then transported throughout the body to fuel our cells and organs.
3. Immune Function
A large portion of the body’s immune system resides in the gut. It acts as a barrier to harmful pathogens, such as bacteria and viruses. A healthy gut microbiome— the community of beneficial bacteria—supports immune function and helps protect the body from infections and inflammation.
4. Detoxification
The gut plays a vital role in detoxifying the body by processing and eliminating waste. The liver, bile, and gut work together to filter out toxins, which are then excreted through the stool. This process helps maintain a clean internal environment.
5. Hormone Regulation
The gut is involved in hormone production and regulation. It helps control hormones related to digestion, hunger, and metabolism. Additionally, the gut microbiome can influence hormonal balance, which is vital for reproductive health.
6. Gut-Brain Connection
The gut and brain communicate through the gut-brain axis, a direct link between the two. This connection influences mood, mental clarity, and stress levels. Research suggests that an imbalance in the gut microbiome can impact mental health conditions like anxiety and depression.
By understanding these basic functions, we can see why maintaining a healthy gut is essential for overall well-being and fertility. Now, let’s dive deeper into how to support these functions for optimal health.
Understanding Gut Permeability and Leaky Gut
Leaky gut occurs when the intestinal barrier becomes compromised, allowing undigested food particles, toxins, and microbes to enter the bloodstream. This process can trigger systemic inflammation and is implicated in conditions like autoimmune diseases, irritable bowel syndrome (IBS), and even neuroinflammation. The protein zonulin regulates tight junctions in the gut lining, and its overproduction is associated with increased gut permeability.
Dietary choices, stress, and environmental toxins all influence this delicate balance.
The Role of Diet in Gut Health
Diet plays a crucial role in shaping gut microbiota and maintaining a strong intestinal barrier. Research suggests that:
- High-fiber foods (e.g., fruits, vegetables, whole grains) support beneficial bacteria and help regulate gut permeability.
- Healthy fats, such as omega-3s, promote anti-inflammatory gut conditions, whereas excessive saturated fat intake can negatively impact gut flora.
- Akkermansia muciniphila, a beneficial bacterium, is linked to improved gut barrier function, reduced inflammation, and better metabolic health.
- Bovine colostrum supplementation has been shown to decrease intestinal permeability and lower zonulin levels, particularly in athletes.
Small Intestinal Bacterial Overgrowth (SIBO) and Gut Dysfunction
SIBO occurs when there’s an overgrowth of bacteria in the small intestine. This can lead to bloating, malabsorption, and digestive discomfort. It’s often associated with IBS, celiac disease, and metabolic syndrome.
Managing SIBO:
- Get proper testing to identify SIBO.
- Modify your diet, focusing on low FODMAP foods.
- Consider probiotics to restore balance.
- Work with a healthcare provider to determine if antibiotics are necessary.
Gut Health and Systemic Wellness
Emerging research highlights the gut-brain connection, linking gut health to cognitive function, mood regulation, and neurological diseases like Alzheimer’s. The gut microbiome also plays a role in cardiovascular health, obesity, and diabetes. Fecal microbiota transplants (FMT) have even been explored as potential treatments for age-related cognitive decline and metabolic disorders.
Gut Health and Fertility
Emerging research suggests that gut health plays a crucial role in reproductive health. The gut microbiome influences hormone regulation, immune function, and inflammation, all of which impact fertility outcomes. Dysbiosis, or an imbalance of gut bacteria, has been linked to conditions like polycystic ovary syndrome (PCOS), endometriosis, and unexplained infertility.
- Hormonal Balance: The gut microbiome helps regulate estrogen levels through the estrobolome, a collection of bacteria involved in estrogen metabolism. An imbalance can lead to estrogen dominance, which is associated with infertility and conditions like PCOS.
- Inflammation and Immune Function: Chronic inflammation, often driven by poor gut health, has been implicated in endometriosis and implantation failure. A healthy gut barrier helps regulate immune responses and supports a favorable reproductive environment.
- Microbiome and Pregnancy Outcomes: Research suggests that a balanced gut microbiome contributes to healthy pregnancy outcomes, reducing the risk of gestational diabetes, preeclampsia, and preterm birth.
Supporting Digestion
Efficient digestion breaks down food properly, allowing for optimal nutrient absorption and minimizing digestive distress.
Ways to enhance digestion include:
- Incorporating bitter foods: Foods like arugula, artichoke, bitter melon, dandelion greens, Brussels sprouts, coffee, and grapefruit stimulate stomach acid and bile production.
- Using digestive aids: Digestive enzymes, HCl supplements, apple cider vinegar, or digestive bitters may be beneficial.
- Relaxing at meals: Stress can negatively impact digestion, so mindful eating practices are essential.
- Consuming adequate minerals: Sodium (from sea salt) and zinc (from oysters and red meat) support stomach acid production.
Supporting Healthy Bile Flow
Bile is critical for fat digestion and detoxification. Signs of inadequate bile include bloating, floating stools, nausea after eating fats, and vitamin deficiencies. To support bile production:
- Consume fiber-rich foods: Legumes, beans, and avocados help bind to excess bile.
- Eat bitter foods: These naturally promote bile flow.
- Use cholagogue herbs: Globe artichoke, dandelion, burdock, and Oregon grape enhance bile movement.
- Ensure adequate taurine intake: Meat, fish, shellfish, and eggs aid in bile salt production.
Supporting Beneficial Bacteria
A balanced gut microbiome is essential for digestion, immunity, and gut barrier integrity. To nurture beneficial bacteria:
- Prioritize digestion first: Ensuring proper food breakdown is key before increasing fiber intake.
- Incorporate prebiotic foods: Apples, asparagus, garlic, onions, oats, and legumes serve as fuel for gut bacteria.
- Limit excessive alcohol intake: Alcohol can cause dysbiosis and inflammation.
Supporting Liver Detoxification
The liver plays a crucial role in gut health through bile production and detox processes. To support liver function:
- Include Phase 1 detox foods: Magnesium (leafy greens, avocado), B vitamins (liver, eggs, seafood), vitamin C (citrus, bell peppers), and zinc (oysters, beef).
- Incorporate Phase 2 detox foods: Glycine (bone broth), glutamine (beef, spinach), cysteine (broccoli, eggs), and taurine (meat, fish).
Strengthening the Gut Lining
A strong intestinal barrier prevents harmful substances from entering the bloodstream. Factors that contribute to a leaky gut include stress, poor digestion, processed foods, overuse of medications, and imbalanced gut bacteria. To support gut integrity:
- Limit inflammatory foods: Avoid heavily processed and inflammatory oils.
- Boost beneficial fibers: Prebiotic and resistant starch-rich foods enhance gut lining health.
- Consume gut-supportive nutrients: Glutamine (cabbage, fish), zinc (beef, crab), and colostrum aid in healing the gut lining.
- Use gut-healing herbs: Marshmallow root, slippery elm, aloe vera, and licorice can be beneficial.
Strengthening the Immune System
A well-functioning immune system relies on strong digestion and a balanced gut microbiome. Factors that deplete immunity include poor digestion, chronic stress, hormonal imbalances, and long-term medication use. To support immune health:
- Improve digestion and gut microbiome health
- Incorporate immune-boosting foods: Colostrum, mushrooms (reishi, shiitake), and vitamin C-rich foods (citrus, mango, papaya) support immune function.
- Use supportive herbs: Andrographis, elderberry, echinacea, and astragalus help strengthen immunity.
Prebiotics & Resistant Starch
Prebiotics are fibers that feed beneficial bacteria and help produce short-chain fatty acids, which support gut integrity and immunity.
- Prebiotic foods: Apples, asparagus, garlic, onions, oats, and legumes.
- Resistant starch sources: Cooked and cooled potatoes, green bananas, and legumes.
By focusing on these key areas, you can create a solid foundation for optimal gut health and overall well-being. Making small, sustainable changes to your diet and lifestyle can have lasting positive effects on digestion, immunity, and energy levels.
Conclusion
Maintaining gut health is essential for overall well-being, from digestion and immunity to mental clarity and chronic disease prevention. By making mindful dietary and lifestyle choices, you can support a resilient gut microbiome and improve long-term health outcomes. The science is clear: a healthy gut is a foundation for a thriving body and mind.

Sources
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6996528/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8305009/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6313445/
- https://pubmed.ncbi.nlm.nih.gov/38790992/
- https://pubmed.ncbi.nlm.nih.gov/32023228/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8058106/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8674859/
- https://pubmed.ncbi.nlm.nih.gov/25290618/
- https://pubmed.ncbi.nlm.nih.gov/35874661/
- https://pubmed.ncbi.nlm.nih.gov/34623232/
- https://www.imrpress.com/journal/FBL/26/5/10.52586/4921/htm
- https://www.nia.nih.gov/news/beyond-brain-gut-microbiome-and-alzheimers-disease
- https://pubmed.ncbi.nlm.nih.gov/34054740/
- https://pubmed.ncbi.nlm.nih.gov/28397754/
- https://pubmed.ncbi.nlm.nih.gov/35745242/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7971312/
- https://pubmed.ncbi.nlm.nih.gov/28778332/

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Cervical health is a vital aspect of women’s overall well-being, encompassing the maintenance of the cervix—the lower, narrow part of the uterus that connects to the vagina. A healthy cervix plays a crucial role in reproductive health, acting as a barrier to infections and facilitating childbirth. While regular medical screenings and vaccinations are essential components of cervical care, adopting natural approaches can further support and enhance cervical health. This article delves into various natural strategies, including nutrition, lifestyle modifications, and herbal remedies, to promote optimal cervical well-being.
Understanding the Cervix
The cervix is a critical structure within the female reproductive system, serving multiple functions that support fertility, pregnancy, and overall gynecological health. It is approximately 2 to 3 centimeters long and is composed of dense connective tissue and smooth muscle. The cervix connects the uterus to the vagina and has a small opening, known as the cervical os, which changes throughout a woman’s life and menstrual cycle.
One of the cervix’s primary functions is to regulate the passage of substances between the uterus and the vagina. The cervical mucus produced by specialized glands within the cervix plays a key role in this process. During ovulation, the mucus becomes thinner and more slippery, facilitating sperm movement toward the egg. In contrast, outside the fertile window, cervical mucus thickens to form a protective barrier that helps prevent infections from ascending into the uterus.
During pregnancy, the cervix undergoes significant changes to support fetal development. It remains firm and closed to keep the developing baby secure in the uterus. In the final weeks of pregnancy, the cervix gradually softens, shortens, and dilates in preparation for labor. This process, known as cervical effacement and dilation, is essential for a smooth delivery.
The cervix also plays a crucial role in protecting against infections. It serves as a physical barrier, preventing harmful bacteria and viruses from entering the uterus. The cervix’s immune response, including the production of antimicrobial proteins and immune cells, helps maintain a balanced vaginal microbiome. An imbalance in the cervical and vaginal microbiota can increase susceptibility to infections such as bacterial vaginosis and sexually transmitted infections (STIs), including human papillomavirus (HPV), which is a major risk factor for cervical cancer.
Cervical health has influence on various factors, including hormonal changes, immune function, and lifestyle choices. Regular Pap smears and HPV tests are essential for detecting early changes in cervical cells that could indicate precancerous conditions. Additionally, maintaining a nutrient-rich diet, avoiding tobacco use, and practicing safe sex can significantly contribute to cervical well-being.
The Role of Nutrition in Cervical Health
A balanced diet rich in specific nutrients can significantly impact cervical health by supporting the immune system, promoting healthy cell function, and reducing the risk of infections and diseases. Research indicates that certain vitamins and minerals are particularly beneficial:
- Vitamin C: Known for its immune-boosting properties, vitamin C enhances collagen production, which maintains cervical tissue integrity. It also acts as an antioxidant, reducing oxidative stress that contributes to cervical abnormalities. Incorporate citrus fruits, bell peppers, strawberries, and broccoli into your diet.
- Beta-Carotene & Vitamin A: These nutrients are essential for epithelial cell health, which includes cervical cells. Vitamin A supports immune function and promotes cell differentiation, reducing the risk of dysplasia. Sources include carrots, sweet potatoes, spinach, and kale.
- Folate (Vitamin B9): Folate plays a critical role in DNA synthesis and repair, reducing the likelihood of abnormal cervical cells. A diet rich in leafy greens, legumes, avocados, and citrus fruits ensures adequate intake.
- Vitamin E: This powerful antioxidant protects cervical cells from oxidative stress and supports reproductive health. Nuts, seeds, spinach, and sunflower oil are excellent sources.
- Zinc: Zinc supports immune function, aids in DNA repair, and promotes healthy cell division. It is found in meats, dairy, nuts, and whole grains.
- Probiotics: A healthy cervical and vaginal microbiome is crucial in preventing infections and maintaining pH balance. Fermented foods such as yogurt, kimchi, and sauerkraut help introduce beneficial bacteria that support immune function.
- Omega-3 Fatty Acids: These essential fats have anti-inflammatory properties that help regulate immune responses and support cell integrity. Sources include fatty fish, flaxseeds, and walnuts.
Incorporating these nutrients into your diet can be achieved by consuming a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats. For instance, a salad with spinach, kale, shredded carrots, and sunflower seeds, accompanied by a citrus-based dressing, can provide a nutrient-dense meal supportive of cervical health.
Foods and Substances to Limit or Avoid
While certain foods can enhance cervical health, others may have detrimental effects and should be consumed in moderation:
- Processed Foods: High levels of preservatives and additives in processed foods can contribute to inflammation and negatively impact overall health.
- Sugary Beverages: Excessive sugar intake is linked to inflammation and an increased risk of infections. Opt for water, herbal teas, or natural fruit juices instead.
- High-Fat Dairy Products: Saturated fats found in high-fat dairy products may negatively affect cellular health and immune function. Choosing low-fat or plant-based dairy alternatives can be beneficial.
- Processed Meats: Diets high in processed meats are found to be associated with increased inflammation and a higher risk of certain cancers. Incorporating plant-based proteins or lean meats can be a healthier alternative.
- Alcohol: Excessive alcohol consumption is linked to an increased risk of cervical cancer and can compromise the immune system. Limiting alcohol intake can help maintain cervical health.
Lifestyle Modifications for Cervical Health
Beyond diet, lifestyle habits play a crucial role in maintaining cervical well-being. Small changes can make a big difference in overall health.
Regular Physical Activity
Engaging in regular exercise helps maintain a healthy weight, reduces stress, and strengthens the immune system. Activities like walking, yoga, or strength training can improve circulation and overall reproductive health.
Avoiding Tobacco Use
Smoking is a significant risk factor for cervical cancer. It weakens the immune system, making it harder for the body to fight off HPV infections. Quitting smoking can dramatically reduce this risk and improve overall well-being.
Practicing Safe Sex
Using condoms and limiting the number of sexual partners can lower the risk of HPV and other STIs. Since HPV is a leading cause of cervical cancer, safe sex practices are vital for prevention.
Managing Stress
Chronic stress weakens the immune system, making the body more susceptible to infections. Stress management techniques such as meditation, yoga, deep breathing exercises, or spending time in nature can promote overall health, including cervical wellness.
Herbal Remedies and Supplements
Traditional practice incorporates herbs and supplements to support cervical health:
- Green Tea: Green tea contains polyphenols, which are antioxidants known for their potential cancer-fighting properties. Regular consumption of green tea may contribute to cervical health by combating oxidative stress and inflammation.
- Turmeric: Curcumin, the active compound in turmeric, has anti-inflammatory and antioxidant properties. Adding turmeric to your diet may help maintain cervical health by reducing inflammation and supporting the body’s defense mechanisms.
- Turkey Tail Mushroom: Turkey tail mushrooms (Coriolus versicolor) are used in traditional Chinese medicine for their immune-boosting properties. They contain polysaccharide K (PSK) and polysaccharopeptide (PSP), which enhance immune health and may help fight HPV infections.
Integrating Functional Nutrition into Daily Life
A practical way to incorporate these nutrients into your daily routine is by creating meals that support cervical health. For instance:
- A smoothie made with spinach, kale, banana, Greek yogurt, and flaxseeds provides essential vitamins, probiotics, and omega-3s.
- A salad with mixed greens, shredded carrots, sunflower seeds, and grilled salmon delivers a nutrient-dense meal that promotes cervical integrity.
- Herbal teas with green tea and turmeric can offer daily antioxidant and anti-inflammatory benefits.
In Closing
Cervical health is a vital component of overall well-being, and taking proactive steps to support it naturally can be highly beneficial. By incorporating a nutrient-rich diet, adopting healthy lifestyle habits, and considering natural remedies, individuals can promote cervical health and reduce the risk of complications. Regular medical check-ups, including Pap smears and HPV testing, remain essential for early detection and prevention. A holistic approach that combines medical care with natural strategies can empower individuals to maintain optimal cervical health throughout their lives.

Sources:
https://pmc.ncbi.nlm.nih.gov/articles/PMC7698010
https://pmc.ncbi.nlm.nih.gov/articles/PMC4997408

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Hormonal contraceptives, including birth control pills, patches, injections, and intrauterine devices (IUDs), have transformed reproductive health, offering women reliable family planning options. However, many individuals experience symptoms after discontinuing hormonal contraception, a phenomenon sometimes referred to as post-birth control syndrome (PBCS). These symptoms can range from irregular cycles and acne to mood swings and digestive issues. Understanding the impact of hormonal contraceptives on the body and implementing strategies to support recovery can help ease this transition.
Understanding the Effects of Hormonal Contraceptives
Hormonal contraceptives work by suppressing ovulation, altering cervical mucus, and changing the uterine lining to prevent pregnancy. While effective, these changes influence several body systems, including the endocrine, digestive, and immune systems. Long-term use can disrupt the body’s natural hormone production, leading to potential withdrawal effects when stopping contraception.
A recent study found that hormonal contraceptives impact the hypothalamic-pituitary-adrenal (HPA) axis, which regulates stress response and hormone production. This may explain why some women experience mood disturbances and fatigue after discontinuation. Additionally, research suggests that birth control pills may alter gut microbiota composition, contributing to inflammation and digestive issues post-contraception.
The Role of the HPA Axis
The HPA axis plays a crucial role in regulating cortisol, a stress hormone that influences metabolism, immune function, and mood. Studies have shown that long-term contraceptive use can disrupt this delicate balance, leading to post-pill anxiety, fatigue, and even adrenal dysfunction. As the body readjusts, individuals may experience heightened stress sensitivity and emotional imbalances.
Additionally, research suggests that chronic hormonal suppression can contribute to reduced ovarian hormone production post-contraception, leading to symptoms like irregular cycles, low libido, and difficulty ovulating.
Common Symptoms After Stopping Hormonal Contraceptives
Post-birth control syndrome encompasses a variety of symptoms that may arise within weeks or months after stopping contraception.
Common symptoms include:
- Irregular or absent menstrual cycles
- Acne and skin changes
- Hair loss or thinning
- Digestive disturbances, including bloating and constipation
- Fatigue and mood swings
- Low libido
- Headaches and joint pain
These symptoms occur as the body attempts to restore natural hormone balance. For some, this transition is seamless, while for others, it may take several months to regulate.
Life After Birth Control: What to Expect
The transition off hormonal contraceptives varies for each individual. Some experience a smooth adjustment, while others face lingering hormonal imbalances.
- Menstrual Cycle Irregularities: It may take several months for cycles to regulate. If cycles remain absent or irregular for more than six months, professional evaluation is recommended. Ovulatory dysfunction is common post-contraception, particularly after long-term use of hormonal birth control. Tracking basal body temperature (BBT) and cervical mucus can provide insight into ovulation status and cycle health
- Acne and Skin Changes: Hormonal shifts can temporarily worsen acne. Supporting detox pathways, reducing dairy and sugar intake, and using non-comedogenic skincare products can help. Elevated androgens post-pill can contribute to excess sebum production, leading to breakouts. Incorporating zinc, omega-3 fatty acids, and antioxidants may promote clearer skin.
- Mood and Energy Levels: Some experience heightened anxiety or depression post-contraception. Prioritizing gut health, sleep, and stress reduction can ease this transition. The gut-brain axis plays a key role in mood regulation, making probiotics and a fiber-rich diet beneficial for mental well-being.
- Fertility Awareness: Some individuals regain fertility immediately, while others need time for ovulation to resume. Those trying to conceive may benefit from monitoring ovulation signs. If fertility does not return within six months, an evaluation for conditions like post-pill PCOS or hypothalamic amenorrhea may be necessary.
- Weight Fluctuations: Water retention and metabolism changes can impact weight. Focusing on whole foods, movement, and hydration supports a stable transition. Hormonal contraceptives can affect insulin sensitivity, and some women notice changes in blood sugar regulation post-pill. Balancing macronutrients and avoiding refined sugars can help stabilize weight.
- Increased Libido: Many report improved libido and natural cycle awareness after stopping hormonal contraceptives due to restored testosterone and estrogen levels.
Adjusting to life after birth control involves patience and self-care. Tracking symptoms, optimizing nutrition, and seeking support when needed can help individuals regain hormonal balance and overall well-being.
Supporting Hormonal Balance Post-Contraception
While post-birth control symptoms can be challenging, several strategies can support the body’s recovery and restore hormonal balance.
1. Nourishing Your Body with Key Nutrients
Hormonal contraceptives can deplete essential nutrients, including B vitamins, magnesium, zinc, and vitamin C. It has been found essential to replenish these nutrients to support metabolism, immune function, and hormone production.
Incorporating the following nutrient-dense foods can be beneficial:
- B Vitamins: Found in leafy greens, eggs, and whole grains
- Magnesium: Present in nuts, seeds, and dark chocolate
- Zinc: Found in oysters, beef, and lentils
- Vitamin C: Abundant in citrus fruits, bell peppers, and strawberries
Supplementing with a high-quality multivitamin or targeted nutrients may also help restore levels more efficiently.
2. Prioritizing Liver Health
The liver plays a crucial role in metabolizing hormones and detoxifying excess estrogen. Supporting liver function can aid hormone clearance and balance. Key strategies include:
- Drinking plenty of water to support detoxification
- Eating cruciferous vegetables (broccoli, cauliflower, kale) to promote estrogen metabolism
- Avoiding alcohol and excessive caffeine, which can burden the liver
- Taking liver-supporting supplements such as milk thistle and dandelion root
3. Balancing Blood Sugar Levels
Insulin resistance and blood sugar imbalances can contribute to hormonal dysregulation post-contraception. Stabilizing blood sugar helps maintain steady energy levels and prevents cortisol spikes, which can further disrupt hormones. To support blood sugar balance:
- Consume protein and healthy fats with every meal
- Avoid refined carbohydrates and excessive sugar
- Incorporate fiber-rich foods, such as legumes, nuts, and vegetables
- Engage in regular physical activity to improve insulin sensitivity
4. Restoring Gut Health
The gut microbiome influences hormone metabolism and immune function. Studies suggest that hormonal contraceptives may alter gut bacteria, leading to digestive issues and inflammation. Supporting gut health can enhance nutrient absorption and hormone clearance:
- Probiotic-Rich Foods: Yogurt, kimchi, sauerkraut, and kefir can replenish beneficial bacteria
- Prebiotic Fiber: Found in onions, garlic, bananas, and asparagus to support microbial diversity
- Bone Broth and Collagen: Aid in gut lining repair
- Limiting Processed Foods: Reducing inflammatory foods can alleviate digestive distress
- Fermented Foods and Fiber: Incorporating fermented foods like miso and fiber-rich foods such as flaxseeds can further support microbiome diversity
According to research, discontinuing birth control can cause shifts in the gut microbiome that affect estrogen metabolism and immune responses. A focus on gut healing post-contraception may accelerate hormonal recovery and reduce systemic inflammation.
5. Managing Stress and Prioritizing Sleep
Chronic stress and inadequate sleep can exacerbate hormonal imbalances. Since the HPA axis is affected by hormonal contraceptives, post-contraceptive recovery requires stress management techniques. Effective strategies include:
- Practicing mindfulness or meditation
- Engaging in gentle movement, such as yoga or walking
- Setting a consistent sleep schedule and avoiding blue light before bedtime
- Taking adaptogenic herbs, like ashwagandha or rhodiola, to support adrenal function
6. Tracking Your Menstrual Cycle
Monitoring menstrual patterns post-contraception provides insight into hormonal recovery. Using a cycle-tracking app or basal body temperature charting can help identify ovulation and cycle health.
- Basal Body Temperature (BBT): Measuring BBT each morning helps detect ovulation. A sustained temperature rise typically indicates ovulation has occurred.
- Cervical Mucus Changes: Observing cervical mucus consistency can signal fertility. Egg-white-like mucus usually indicates peak fertility.
- Cycle Length and Symptoms: Keeping track of cycle length, PMS symptoms, and flow characteristics provides valuable data about hormonal balance.
- Ovulation Predictor Kits: These kits measure luteinizing hormone (LH) surges, indicating the fertile window.
If menstruation does not return within three to six months, consulting a healthcare provider may be necessary to rule out underlying conditions like hypothalamic amenorrhea or PCOS.
7. Seeking Professional Support
If symptoms persist or become severe, working with a healthcare provider, such as a functional medicine/nutrition practitioner, can be beneficial. They can assess hormone levels, address underlying imbalances, and provide personalized recommendations for recovery.
Here are some issues you may need to address:
Prolonged Absence of Periods: If your period hasn’t returned after six months.
Persistent Acne or Severe Hair Loss: Significant changes in skin or hair health could indicate hormonal imbalances that require attention.
Excessive Mood Changes or Fatigue: If symptoms like mood swings, anxiety, or extreme tiredness persist.
Chronic Digestive Issues: Ongoing digestive disturbances such as bloating or constipation.
Conclusion
Recovering from hormonal contraceptives is a unique process for every individual. While some may transition smoothly, others may experience a range of symptoms as their body readjusts. By focusing on nutrient replenishment, liver and gut health, blood sugar balance, stress management, and cycle tracking, individuals can support their hormonal recovery more effectively. If challenges persist, seeking professional guidance can ensure a smoother transition and optimal long-term health.

Sources:
https://drbrighten.com/post-birth-control-syndrome
https://drbrighten.com/stopping-birth-control-side-effects
https://www.sciencedirect.com/science/article/pii/S0889159123003331?via%3Dihub
https://pmc.ncbi.nlm.nih.gov/articles/PMC6055351
https://drbrighten.com/the-contraception-guide/ https://www.kernodle.com/obgyn_blog/side-effects-of-stopping-the-pill-after-prolonged-use/

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
If you’re trying to conceive, the food on your plate might be more important than you think! The link between diet and fertility is stronger than ever, with research showing that the right nutrition can make all the difference in hormone balance, egg and sperm quality, and overall reproductive health. Enter the Modified Mediterranean Diet – an upgraded version of one of the world’s healthiest eating patterns, tailored specifically for fertility support. Packed with antioxidants, healthy fats, and essential nutrients, this approach can help set the stage for a successful pregnancy. Let’s dive into how you can use food as a powerful tool to enhance fertility naturally!
The Role of Nutrition in Fertility
What you eat plays a direct role in shaping your reproductive health. A well-balanced diet provides the essential nutrients needed for hormone production, optimal egg and sperm quality, and a healthy reproductive system. Poor dietary choices, on the other hand, can lead to inflammation, oxidative stress, and metabolic imbalances, all of which can impair fertility.
One of the key factors in fertility is oxidative stress, which occurs when free radicals damage cells, including eggs and sperm. Antioxidant-rich foods such as berries, leafy greens, and nuts help neutralize these harmful compounds, protecting reproductive cells and improving their function. Research has shown that a diet high in antioxidants is linked to improved sperm motility and morphology, as well as better ovarian function in women.
Another crucial aspect is hormonal balance. Hormones like estrogen, progesterone, and testosterone rely on a steady supply of vitamins and minerals to function properly. Nutrients such as zinc, vitamin D, and omega-3 fatty acids support hormone synthesis and regulation, helping to optimize fertility. Consuming high-quality protein sources, healthy fats, and fiber-rich carbohydrates helps maintain stable hormone levels and reduces the risk of conditions like polycystic ovary syndrome (PCOS), which is a leading cause of infertility.
Additionally, mitochondrial health plays a significant role in reproductive success. Mitochondria, known as the powerhouses of the cell, provide the energy needed for fertilization and embryo development. Nutrients like CoQ10, found in fish, nuts, and organ meats, support mitochondrial function, ensuring that eggs and sperm have the energy required for optimal performance.
Finally, blood sugar stability is vital for fertility. High blood sugar levels can disrupt ovulation, impair egg quality, and contribute to insulin resistance, which is commonly associated with PCOS. A diet that prioritizes low-glycemic carbohydrates, lean proteins, and healthy fats can help regulate blood sugar levels and improve overall reproductive health.
By focusing on nutrient-dense foods that combat oxidative stress, support hormone production, enhance mitochondrial function, and stabilize blood sugar, you can create the best possible environment for conception and a healthy pregnancy.
Why the Modified Mediterranean Diet?
The Mediterranean diet has long been associated with numerous health benefits, including improved heart health, reduced inflammation, and better metabolic function. Studies have found that adherence to a Mediterranean diet is linked to increased fertility, improved assisted reproductive technology (ART) outcomes, and better pregnancy success rates.
However, for optimal fertility benefits, modifications to the traditional Mediterranean diet can enhance its effects. A modified Mediterranean diet prioritizes lower glycemic load foods, nutrient-dense proteins, and specific fertility-enhancing nutrients.
Understanding Glycemic Index vs. Glycemic Load
People often hear about glycemic index (GI) and glycemic load (GL) when discussing blood sugar management, but they are not the same. The glycemic index measures how quickly a carbohydrate-containing food raises blood sugar on a scale from 0 to 100. However, it does not account for portion size. Glycemic load, on the other hand, considers both the GI and the amount of carbohydrates in a typical serving, giving a more accurate picture of a food’s impact on blood sugar. For fertility, focusing on low glycemic load foods is more beneficial for stabilizing blood sugar and hormone balance.
Read more about how to balance blood sugar through your meals here.
Key Components of the Modified Mediterranean Diet
1. Healthy Fats for Hormone Balance
Healthy fats play a vital role in hormone production and cell membrane integrity. The modified Mediterranean diet emphasizes:
- Extra virgin olive oil
- Avocados
- Nuts and seeds (e.g., walnuts, flaxseeds, almonds)
- Omega-3-rich fatty fish (e.g., salmon, sardines, mackerel)
- Grass-fed animal fats in moderation
These fats support reproductive hormone function and reduce inflammation, benefiting egg and sperm quality.
2. High-Quality Protein Sources
Protein is essential for reproductive health, but the source matters. This diet focuses on:
- Grass-fed beef and pasture-raised poultry
- Wild-caught fish
- Eggs (rich in choline and vitamin B12)
- Legumes and lentils
- Full-fat dairy (linked to improved ovulation in women with PCOS)
Protein from high-quality sources supports mitochondrial function in eggs and sperm and provides key amino acids necessary for hormone production.
3. Antioxidant-Rich Foods
Oxidative stress is a significant contributor to poor egg and sperm quality. The modified Mediterranean diet is rich in antioxidants that combat free radical damage:
- Berries (blueberries, raspberries, strawberries)
- Dark leafy greens (spinach, kale, Swiss chard)
- Cruciferous vegetables (broccoli, Brussels sprouts)
- Herbs and spices (turmeric, ginger, rosemary)
A diet high in antioxidants has been shown to improve sperm motility and morphology while enhancing egg quality.
4. Low-Glycemic Carbohydrates
Blood sugar imbalances can negatively impact fertility, particularly in individuals with insulin resistance or PCOS. This diet reduces refined grains and includes:
- Quinoa, farro, and barley in moderation
- Sweet potatoes, squash, and beets
- Legumes and lentils for fiber and protein
Stabilizing blood sugar through a low-glycemic diet helps regulate ovulation and improve egg quality.
5. Essential Micronutrients for Fertility
Several key vitamins and minerals are essential for reproductive health:
- Folate & B Vitamins: Support methylation and DNA synthesis (found in leafy greens, beans, and liver).
- Vitamin D: Linked to improved ovarian function and implantation (from sunlight, fatty fish, and fortified dairy).
- Zinc: Essential for sperm production and egg maturation (in nuts, seeds, and shellfish).
- CoQ10: Supports mitochondrial function in eggs and sperm (in grass-fed meat, fish, and supplements).
- Choline: Crucial for fetal brain development and egg quality (in eggs and liver).
Learn more about my recommendations for prenatal supplements here.
Practical Meal Ideas for Fertility Support
To make following this diet easier, here are additional meal ideas:
Breakfast:
- Greek yogurt parfait with walnuts, chia seeds, and fresh berries.
- Scrambled eggs with sautéed spinach, tomatoes, and feta cheese on whole-grain toast.
- Oatmeal with almond butter, flaxseeds, and a sprinkle of cinnamon.
Lunch:
- Grilled salmon with quinoa, steamed asparagus, and a drizzle of olive oil.
- Mediterranean chickpea salad with cucumbers, cherry tomatoes, red onion, feta cheese, and olive oil dressing.
- Lentil soup with a side of whole-grain bread and a mixed greens salad.
Dinner:
- Grass-fed steak with sweet potato mash and roasted Brussels sprouts.
- Baked cod with a side of roasted vegetables (zucchini, bell peppers, eggplant) and brown rice.
- Chicken and vegetable stir-fry with cauliflower rice and sesame ginger dressing.
Snacks:
- Hummus with carrot and celery sticks.
- A handful of almonds and dark chocolate.
- Cottage cheese with flaxseeds and sliced peaches.
- Hard-boiled eggs with a sprinkle of sea salt.
Lifestyle Considerations for Fertility
In addition to diet, lifestyle factors play a crucial role in optimizing fertility:
- Stress Management: Chronic stress disrupts hormonal balance. Incorporate mindfulness, yoga, or meditation.
- Sleep Hygiene: Poor sleep affects hormone regulation. Aim for 7-9 hours of quality sleep per night.
- Exercise: Moderate exercise improves fertility, but excessive exercise can have negative effects, particularly on ovulation.
- Reducing Toxins: Minimize exposure to endocrine disruptors such as BPA and phthalates found in plastics and personal care products.
Research Insights and Case Studies
Several studies highlight the success of dietary modifications in improving fertility:
- Women who adhered to a Mediterranean-style diet had a 65% higher chance of conception through IVF.
- A study found that men following a nutrient-rich diet improved their sperm parameters within just three months.
- Higher adherence to the Mediterranean diet was associated with a 40% lower risk of ovulatory infertility in women.
- Couples undergoing fertility treatments who followed a Mediterranean-style diet had a 30% higher live birth rate compared to those who did not.
- A study on male fertility found that men with a diet rich in antioxidants and omega-3 fatty acids had 20% higher sperm motility and 15% better morphology than those consuming a Western-style diet.
- Women who consumed higher levels of folate and vitamin B12 had a 50% lower risk of miscarriage compared to those with lower intake.
Conclusion
A modified Mediterranean diet offers a comprehensive and evidence-based approach to improving fertility. By emphasizing nutrient-dense foods, balancing blood sugar, and supporting mitochondrial function, this dietary pattern can enhance reproductive health for both men and women. Coupled with a healthy lifestyle, these dietary modifications can significantly improve conception outcomes and pave the way for a healthy pregnancy.
Fertility is a complex journey, and while diet alone may not guarantee success, it plays a crucial role in creating the best possible conditions for conception. Every small change—whether it’s adding more antioxidant-rich foods, choosing high-quality proteins, or reducing processed carbohydrates—can have a profound impact on reproductive health.
If you’re trying to conceive, consider incorporating these dietary principles into your daily routine. Start by making simple swaps, such as using extra virgin olive oil instead of processed vegetable oils or choosing whole grains over refined grains. Focus on consuming a variety of colorful fruits and vegetables, lean proteins, and healthy fats. Additionally, be mindful of lifestyle factors such as stress management, sleep quality, and physical activity, all of which influence fertility.
Now is the time to take charge of your fertility health! Whether you’re planning to conceive soon or in the future, these dietary and lifestyle changes can set the foundation for a healthier pregnancy and baby. If you need personalized guidance, consider working with a nutritionist or healthcare professional specializing in fertility nutrition to tailor a plan that meets your unique needs.
Start today—your future self (and baby) will thank you!

Sources
https://pmc.ncbi.nlm.nih.gov/articles/PMC8909876
https://pmc.ncbi.nlm.nih.gov/articles/PMC2846864
https://pmc.ncbi.nlm.nih.gov/articles/PMC4475051
https://pmc.ncbi.nlm.nih.gov/articles/PMC10005661

The Preconception Playbook
This free playbook provides specific actionable tips to get started on your fertility journey, as well as what to avoid while you're trying to conceive.
Get the free playbook