Fertility
Resources
Style
Planning
View All
If you’ve ever been told “everything looks normal”-yet nothing feels normal at all- you know how deeply frustrating those words can be.
You watch friends, coworkers, even strangers announce pregnancies that seemed to happen effortlessly. Meanwhile, you’re tracking, testing, timing and doing everything under the sun… and still, nothing. It’s exhausting. It’s isolating. It can make you feel like you’re somehow missing something obvious.
You’re not.
So many couples reach this same breaking point after hearing that familiar line, “everything looks fine.” It can feel like the end of the road- like the doctors have checked their boxes and moved on, even though your gut tells you something isn’t adding up. Because if everything were truly fine, this wouldn’t feel so hard.
Hormone testing can be incredibly helpful. It gives us a valuable snapshot of what’s happening beneath the surface, at the microscopic level. But here’s the truth, hormones don’t tell the whole story.
Fertility isn’t controlled by a single switch or dictated by hormones alone. It’s a complex, multi-factorial system influenced by far more than any one lab result can capture. When something feels off, it’s worth looking deeper- because “normal” doesn’t always mean optimal, and it certainly doesn’t mean your experience isn’t valid.
What does “normal” hormone blood work actually mean?
When it comes to fertility, hormones are the behind-the-scenes directors calling the shots. But which hormones actually matter- and when should they be tested? Let’s break it down.
Key players we look at for fertility include follicle-stimulating hormone (FSH), luteinizing hormone
(LH), estradiol (E2), anti-Müllerian hormone (AMH), and Progesterone. Together, these hormones
help paint a clear picture of ovarian reserve and overall reproductive function. Most of these labs are checked on day 3 of your menstrual cycle, and that timing isn’t random. Day 3 of your cycle is when many of these hormones are at their lowest, or most baseline, levels. Testing consistently on this day allows us to compare apples to apples each month. Without that consistency, hormone levels can jump all over the chart, making us compare apples to oranges

The “normal” reference ranges you see on lab reports aren’t always the same as optimal ranges for
fertility. Those reference ranges are designed to catch diseases or major deficiencies -not to tell us
whether your body is operating at peak reproductive potential. So yes, you can fall within the “normal” range and still have room for improvement when it comes to fertility.
In short: the right hormones, the right timing, and the right interpretation make all the difference when it comes to understanding your fertility.
Why can Standard labs miss fertility root causes?
As mentioned earlier, the cornerstone hormones assessed in routine fertility testing include
follicle-stimulating hormone (FSH), luteinizing hormone (LH), estradiol (E2), anti-Müllerian
hormone (AMH), and Progesterone. These labs are undeniably important and offer valuable insight into reproductive function. But fertility is far more nuanced than a handful of numbers on a lab report- and there are critical factors these values simply can’t capture.
Blood sugar regulation plays a foundational role in fertility. When blood sugar is poorly controlled,
insulin levels can remain chronically elevated, disrupting hormonal balance. High insulin has been shown to impair egg maturation in women and reduce both sperm count and quality in men. In other words, stable blood sugar isn’t just about energy- it’s about creating the right hormonal environment for conception.
Another major, yet often overlooked, factor is chronic inflammation. Persistent inflammation interferes with hormone signaling, which can lead to irregular ovulation and compromised egg quality. Over time, it may even contribute to structural issues such as uterine scar tissue resulting from chronic pelvic inflammation. For men, chronic inflammation creates a hostile environment for sperm, increasing oxidative stress and impairing healthy sperm development.
Nutrient status is equally essential. Both undernutrition and overnutrition can negatively impact fertility. Undernutrition- often associated with calorie restriction and vitamin deficiencies- is typically more commonly recognized. However, overnutrition- frequently linked to obesity- can coexist with significant micronutrient deficiencies as well. Evaluating and correcting nutrient imbalances is critical not only for conception but also for supporting a healthy pregnancy and baby.
Then there’s gut health, a keystone in hormone balance and nutrient absorption. The gut is far more than just the stomach- it’s an intricate system extending from the mouth to the anus, housing trillions of beneficial bacteria. These microbes play a vital role in extracting, absorbing, and even synthesizing key nutrients. When the gut microbiome is out of balance, nutrient deficiencies and poor digestion often follow. Even more importantly, the gut actively interacts with sex hormones like estrogen, testosterone, and estradiol. When gut function is compromised, hormone imbalances- and fertility challenges- often follow.
By now, a clear theme may be emerging: fertility is deeply interconnected with nearly every aspect of our physiology. This is especially true when it comes to stress. Stress isn’t just an uncomfortable mental state-it triggers real, measurable physiological changes. Chronic stress activates the release of “fight or flight” hormones like cortisol and adrenaline. These can disrupt our overall hormonal balance and negatively affect fertility. Stress can also impair gut health and increase unhealthful coping behaviors such as overeating, excessive alcohol consumption, or smoking-all of which further hinder reproductive health.
To make a long story short, optimizing fertility requires looking beyond hormone labs alone. It means supporting the body as a whole. Balancing blood sugar, calming inflammation, replenishing nutrient stores, healing the gut, and managing stress- so our sex hormones can have the space to do what they need to do.
Can you ovulate and still have hormone dysfunction?

While ovulation is a crucial milestone for fertility, it’s only one piece of a much larger hormonal puzzle. A healthy pregnancy depends not just on releasing an egg, but on creating the ideal environment for that egg to implant and thrive. One of the most critical factors here is the uterine lining. For an embryo to successfully implant, the uterine wall must be thick, nourished, and stable. The hormone responsible for maintaining this environment is progesterone. If progesterone isn’t operating in sufficient amounts, the uterine lining will not be thick enough to sustain a successful implantation.
Timing matters just as much as hormone levels themselves. A well-orchestrated menstrual cycle requires precise communication between hormones. It is critical that the luteal phase, the phase of the menstrual cycle after ovulation, is at least 10 days long. Any time shorter than this is not enough time for progesterone to thicken the uterine wall to sufficient amounts.
Conditions like polycystic ovarian syndrome (PCOS) illustrate this clearly. Some women with PCOS do ovulate regularly, yet continue to experience hormonal imbalance with elevated testosterone levels. Symptoms like acne, excess hair growth, and weight gain can persist despite ovulation, signaling that the underlying hormonal landscape is still out of balance.
The same holds true for thyroid disorders. Both hypothyroidism and hyperthyroidism can disrupt
menstrual cycles and make conception more challenging. And yet, regular ovulation can still occur in both conditions. Once again, ovulation alone doesn’t guarantee optimal fertility.
So in short, Yes- it’s absolutely possible to ovulate and still have hormonal imbalances.
What tests look deeper than standard OB labs?
To gain meaningful insight into fertility, we need to look beyond a single lab panel and take a more
comprehensive, whole-body approach. Utilizing a range of advanced and functional laboratory tests allows us to better understand what’s happening at the microscopic level.
These assessments may include functional blood work, gut testing, mineral analysis, and hormone
metabolism testing. Each test adds another layer of clarity which can help to reveal hidden imbalances that standard testing often misses.
What should I focus on if my labs are “normal”, but I’m not pregnant?
Sometimes all the tests come back “normal”, yet the outcome you’re hoping for still doesn’t happen. If you’ve been there, you know how deeply frustrating- and confusing- that can feel.
When this happens, the next step is often to return to the foundations of health. Supporting fertility starts with making sure your body has enough fuel to run a full, healthy menstrual cycle. That means eating enough- especially the nutrients your hormones rely on to function and communicate effectively.
Nutrition plays a powerful role here. Focusing on gut-supportive foods like fiber-rich beans, whole
grains, and produce. Alongside probiotics like fermented foods can help to nourish the beneficial bacteria within our GI tract. At the same time, reducing artificial sugars supports blood sugar balance and helps to prevent the overgrowth of less-than-healful gut microbes.

Stress management is another key piece of the puzzle. Finding healthy ways to cope during stressful seasons allows your body to spend less time stuck in “fight or flight” mode and more time in a calm, hormonally optimized state. Fertility thrives in an environment of safety and balance.
Finally, this is not a journey meant to be navigated alone. Working with a practitioner who looks at the entire picture, not just a single lab value or isolated symptom, makes all the difference. Fertility is complex, and having someone who understands how all the pieces connect is often the missing link.
Want to learn more?
If you like what you read here, want to know more, but don’t have the time to sit down and read through all our blogs, check out our free private podcast where we break down fertility root causes in more detail. Perfect for those who want to learn more about their hormones and bodies all while still keeping up their busy schedule.
Sources
https://www.stonybrookmedicine.edu/islandfertility/news/sugar
https://rep.bioscientifica.com/view/journals/rep/169/4/REP-24-0197.xml
https://pmc.ncbi.nlm.nih.gov/articles/PMC10097215/
https://azgyn.com/blog/fertility-gut-health

Pregnancy is a season when your body simply needs more—more rest, more support, and yes, more nutrients. During this time, demands for key nutrients like folate, iodine, choline, and vitamin D increase significantly. If these needs aren’t met, deficiencies can have long-term effects not only for you, but for your growing baby as well.
Nourishing your body during this incredibly important and transformative time isn’t optional—it’s foundational to supporting a healthy pregnancy.
Is a healthy diet enough?
Even when you’re eating a well-balanced, nutrient-dense diet, it can still be difficult to meet all of your increased nutrient needs during pregnancy through food alone. This is where a high-quality prenatal vitamin becomes an essential part of your pregnancy toolkit.
Let’s break down a few of the most important nutrients to look for—and why they matter.

Folate
Folate (vitamin B9) is a critical micronutrient for fetal brain and spinal cord development. In the very early weeks of pregnancy—often before someone even knows they’re pregnant—the neural tube forms and closes, eventually developing into the brain and spinal cord. This process typically happens within the first 3–4 weeks of pregnancy.
Folate plays a central role in this process by supporting rapid cell growth and division, as well as methylation—a biochemical process that is essential for proper neural tube closure and healthy brain and spinal cord development.
A quick (and gentle!) biochemistry moment—bear with us. Many supplements and fortified foods use folic acid, which is a synthetic form of vitamin B9. Folic acid must be converted in the body to its active form, methylfolate, before it can be fully utilized. Some individuals have a harder time completing this conversion, which can lead to less-than-optimal absorption.
To bypass this conversion step altogether and support optimal absorption, it’s ideal to choose a prenatal that contains methylfolate rather than folic acid.
Current Recommended Dietary Allowances (RDAs) in the U.S. are:
- 400 mcg/day for women of childbearing age who are not pregnant
- 600 mcg/day for pregnant women
Iodine
Iodine is a crucial micronutrient for thyroid health and function. If you want a deeper dive into iodine’s role in fertility, thyroid health, reproductive health, and hormone balance, be sure to check out our earlier blog: Iodine and Women’s Health: What You Need to Know.
When it comes to pregnancy, iodine deserves special attention. It plays a key role in fetal brain and nervous system development, as well as in thyroid hormone production and regulation for both mom and baby.
The current RDAs in the U.S. are:
- 150 mcg/day for women of childbearing age who are not pregnant
- 220 mcg/day for pregnant women
Because iodine intake varies widely based on diet and food sourcing, it’s an especially important nutrient to confirm is included in your prenatal.

Vitamin D and Calcium
Calcium is essential for bone health, and during pregnancy, needs increase to support fetal skeletal development. At the same time, adequate calcium intake helps protect and maintain mom’s own calcium stores.
During breastfeeding, approximately 3–5% of a mother’s calcium stores can be depleted through breast milk production. While these losses haven’t been directly linked to an increased risk of osteoporosis later in life, ensuring adequate calcium intake before, during, and after pregnancy is still incredibly important.
One of the best ways to support calcium absorption? Vitamin D.
Vitamin D is a fat-soluble vitamin that plays a role in fetal immune system development, overall fetal growth, and—importantly—calcium absorption.
Without getting too deep into the weeds, the active form of vitamin D (calcitriol) helps activate receptors in the intestines that increase the production of calcium-transporting proteins. These proteins work together to improve calcium absorption into the bloodstream—essentially helping your body actually use the calcium you’re consuming.
Current RDAs in the U.S.:
- Calcium: 1000–1300 mg/day (pregnant and non-pregnant women)
- Vitamin D: 15 mcg/day (pregnant and non-pregnant women)
Many perinatal practitioners recommend higher levels of vitamin D for optimal lab levels.
So… which prenatal should I choose?
Understanding nutrient needs is one thing—actually choosing a prenatal is another. With so many options on the market, it’s no wonder this step feels overwhelming.
One important thing to know: many prenatals still rely on outdated RDAs that were originally based on research conducted in men’s bodies—not women’s, and certainly not pregnant women’s.
This is where Needed stands out.
Needed recognized this gap and created prenatals that are science-backed and designed with women’s unique needs in mind—especially during preconception, pregnancy, and postpartum, when nutrient demands are higher across the board.
Needed Prenatal Multi provides 5x more nutrition than outdated RDAs, helping better meet the increased nutrient demands of pregnancy.*
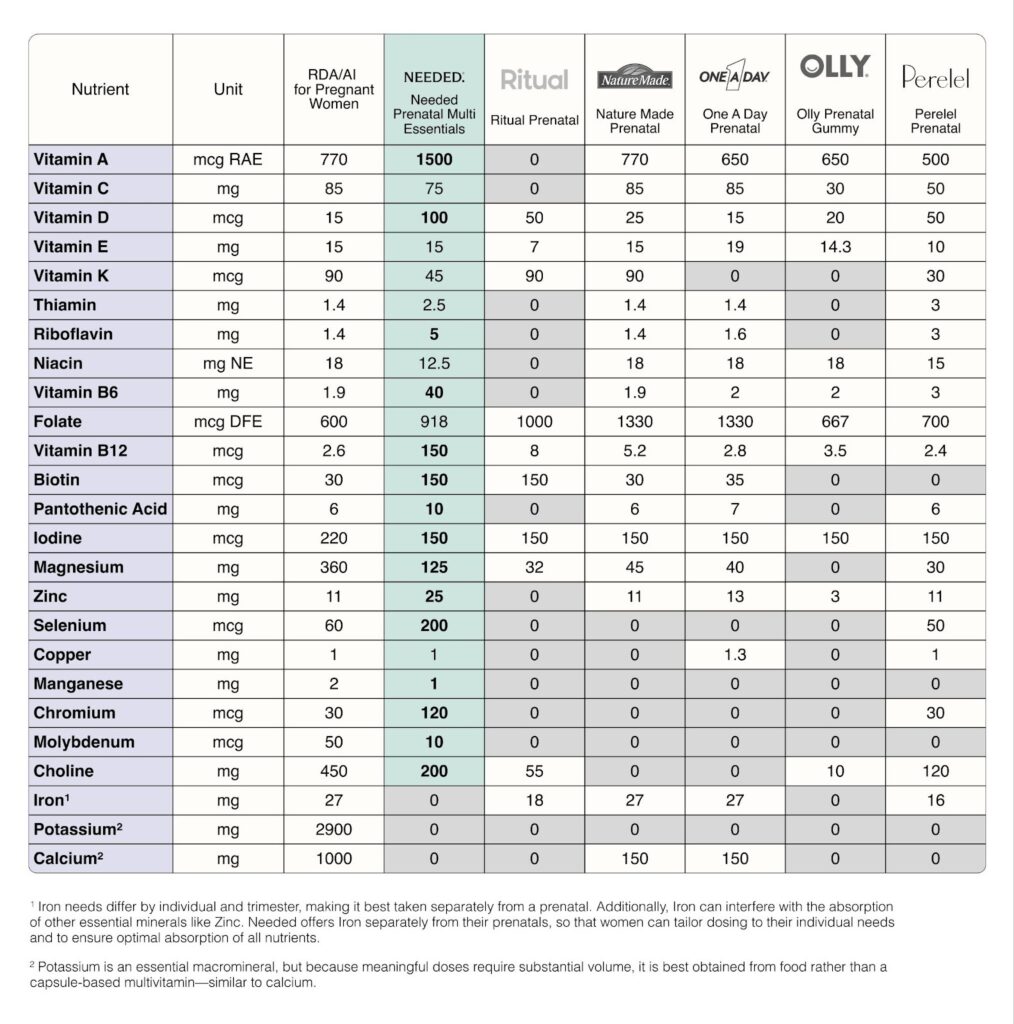
How does Needed compare to other prenatals?

Needed Prenatal Multi Essentials delivers *8x more nutrition than other leading prenatals on the market.
It includes 551 mcg of folate in the methylated form, to support healthy neural tube development and methylation..
And yes—it really is that good.
Needed prenatals are third-party tested, meaning an independent, unbiased organization verifies the safety, quality, and accuracy of all label claims. In short: what’s on the label is exactly what’s in the product.
Needed offers multiple prenatal options: capsules and a vanilla powder, so you can choose what works best for you. I used the vanilla powder during my first pregnancy when I simply couldn’t swallow any pills and it was such a game changer for me personally.
You can easily purchase Needed prenatals directly through their website:
https://thisisneeded.com/products/prenatal-multi-essentials
Looking for More Support?
Navigating prenatal nutrition—and figuring out how to best support both you and your baby—can feel confusing. You don’t have to do this alone.
Using every tool available to you, including personalized nutrition guidance and high-quality supplementation, is one of the simplest ways to support a healthy pregnancy. Our 1:1 coaching services are designed to be that extra layer of support—someone firmly in your corner.
Let’s do this together. Reach out today to begin your journey toward nourishing and supporting your growing life with expert guidance every step of the way.
This post is sponsored by Needed, a brand I genuinely recommend to my patients and personally use.
These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease.
*Based on the total daily dosage of nutrients provided compared to leading prenatals as determined by IRI sales data as of December 2025
Sources:
https://ods.od.nih.gov/factsheets/Folate-HealthProfessional/
https://pmc.ncbi.nlm.nih.gov/articles/PMC4933077/
https://ods.od.nih.gov/factsheets/Iodine-HealthProfessional/
https://www.niams.nih.gov/health-topics/pregnancy-breastfeeding-and-bone-health

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Dealing with endometriosis is already a challenge—pain, fatigue, and the frustratingly long journey to diagnosis. But for many, one of the hardest realities to face is how this condition might impact fertility. Whether you’re actively trying to conceive or simply thinking about the future, it’s natural to wonder: Will I be able to get pregnant? Will it take longer? Am I at risk for complications?
Let’s break it down—why does endometriosis make conception more difficult? And what can be done to improve fertility outcomes?
Fertility and Endometriosis: The Numbers
Studies suggest that up to 50% of people with endometriosis may experience fertility challenges, and about half of those diagnosed with infertility have underlying endometriosis. However, a diagnosis doesn’t mean pregnancy is impossible! It may take longer, require medical support, or necessitate lifestyle adjustments—but many people with endometriosis go on to conceive and carry healthy pregnancies.
Now that we’ve covered the statistics, let’s explore why endometriosis affects fertility in the first place.
Understanding the Connection: Why Endometriosis Affects Fertility
Endometriosis is a complex condition where tissue similar to the uterine lining grows outside the uterus, leading to inflammation, scarring, and hormonal imbalances. These factors can contribute to fertility struggles in multiple ways:
1. Chronic Inflammation and Hormonal Imbalances
Endometriosis is associated with chronic inflammation, which plays a key role in fertility challenges. The condition causes an increase in inflammatory cytokines—proteins that regulate immune responses. These cytokines can interfere with ovulation, fertilization, and implantation by creating a hostile uterine environment. Chronic inflammation may also impair the function of the corpus luteum, the structure responsible for producing progesterone after ovulation. Since progesterone is critical for preparing the uterine lining for implantation, low levels may result in implantation failure or early miscarriage.
Additionally, endometriosis is often linked to estrogen dominance. Excess estrogen can thicken the endometrial lining abnormally, disrupt the menstrual cycle, and contribute to a suboptimal hormonal balance for conception.
2. Reduced Egg Quality and Oxidative Stress
Endometriosis has been linked to oxidative stress, a condition where an excess of reactive oxygen species (ROS) damages cellular structures, including eggs. This oxidative damage can lead to:
- DNA fragmentation in eggs, reducing their ability to be fertilized.
- Lower embryo quality, decreasing the likelihood of successful implantation.
- Higher rates of aneuploidy (chromosomal abnormalities), which can lead to failed pregnancies or birth defects.
Research suggests that targeted nutritional strategies, such as increasing antioxidant intake (e.g., vitamin C, vitamin E, and CoQ10), can help mitigate oxidative stress and improve egg quality.
3. Decreased Ovarian Reserve and Endometriomas
Many individuals with endometriosis develop ovarian cysts known as endometriomas. These cysts, filled with old blood, can impact ovarian function in several ways:
- Damage to ovarian tissue: As endometriomas grow, they can infiltrate and compromise healthy ovarian tissue, reducing the number of viable eggs.
- Lower response to fertility treatments: Studies indicate that individuals with endometriomas often have a lower ovarian response to stimulation during assisted reproductive technologies (ART) like in vitro fertilization (IVF).
- Surgical risks: While surgical removal of endometriomas may relieve symptoms, it can also reduce ovarian reserve if healthy ovarian tissue is inadvertently removed during the procedure. Those considering surgery should discuss fertility preservation strategies, such as egg freezing, beforehand.
4. Blocked Fallopian Tubes and Pelvic Adhesions
Endometriosis can cause adhesions—bands of fibrous scar tissue that develop between organs. These adhesions may:
- Block or distort the fallopian tubes, preventing eggs from traveling to meet sperm.
- Interfere with ovulation, making it more difficult for the ovaries to release eggs effectively.
- Cause fluid buildup in the fallopian tubes (hydrosalpinx), which can create an inhospitable environment for embryos and decrease implantation success.
For those with significant tubal damage, natural conception may be challenging, and assisted reproductive technologies like IVF may be necessary.
5. Implantation Challenges and Uterine Dysfunction
Successful pregnancy depends on a fertilized egg implanting into a healthy uterine lining. Endometriosis can interfere with this process due to:
- Abnormal endometrial receptivity: The endometrium (uterine lining) may not develop properly due to chronic inflammation, hormonal imbalances, or scarring.
- Increased uterine contractility: The uterus may contract excessively, making it harder for an embryo to implant and remain stable.
- Altered immune response: Inflammatory and immune factors in the uterine environment may mistakenly attack the embryo, leading to implantation failure or early miscarriage.
Pregnancy with Endometriosis: Risks & Considerations
While many individuals with endometriosis achieve healthy pregnancies, it’s important to be aware of potential risks and considerations:
1. Increased Risk of Obstetrical Complications
Studies have identified a higher incidence of certain complications in pregnant individuals with endometriosis:
- Preterm Birth: There is an elevated risk of delivering before 37 weeks of gestation.
- Placenta Previa: The placenta may implant low in the uterus, covering the cervix, which can lead to bleeding and necessitate a cesarean section.
- Hypertensive Disorders: Conditions like preeclampsia, characterized by high blood pressure and potential damage to other organ systems, are more common.
- Gestational Diabetes: An increased likelihood of developing diabetes during pregnancy has been observed.
- Cesarean Delivery: The necessity for cesarean sections is higher among those with endometriosis.
These findings underscore the importance of vigilant prenatal care for individuals with endometriosis to monitor and manage potential complications effectively.
2. Impact of Surgical Treatment on Pregnancy Outcomes
Surgical interventions for endometriosis, such as laparoscopic excision, aim to alleviate symptoms and improve fertility. However, the effects of surgery on pregnancy outcomes are complex:
- Adhesion Formation: Post-surgical adhesions can lead to chronic pelvic pain and may impact fertility.
- Ovarian Reserve: Surgical removal of endometriomas (ovarian cysts associated with endometriosis) can reduce ovarian reserve, potentially affecting fertility.
Therefore, surgical decisions should be individualized, weighing the benefits against potential risks, and discussed thoroughly with a healthcare provider.
3. Importance of Preconception Counseling
Given the potential challenges associated with endometriosis and pregnancy, preconception counseling is highly recommended. This process involves:
- Comprehensive Evaluation: Assessing the extent of endometriosis and its impact on reproductive organs.
- Fertility Assessment: Evaluating ovarian reserve and tubal patency to determine the best conception strategies.
- Risk Discussion: Understanding the potential obstetrical risks and planning appropriate monitoring and interventions.
Engaging in preconception counseling allows for informed decision-making and the development of a tailored care plan to optimize pregnancy outcomes.
4. Nutritional and Lifestyle Modifications
Adopting specific dietary and lifestyle changes can positively influence fertility and pregnancy outcomes in individuals with endometriosis:
- Anti-Inflammatory Diet: Consuming foods rich in antioxidants can reduce oxidative stress and improve egg quality.
- Regular Physical Activity: Engaging in moderate exercise can enhance overall health and reduce inflammation.
- Stress Management: Incorporating stress-reduction techniques like yoga or meditation may improve hormonal balance.
Implementing these modifications can support reproductive health and may increase the likelihood of a successful pregnancy.
5. Assisted Reproductive Technologies (ART)
For those experiencing difficulty conceiving naturally, ART options such as in vitro fertilization (IVF) may be considered. While endometriosis can impact the success rates of ART, individualized treatment protocols and close monitoring can enhance outcomes. Consulting with a fertility specialist can provide personalized guidance on the most appropriate interventions.
Ultimately, while endometriosis can pose challenges to conception and pregnancy, understanding the potential risks and proactively managing them with a healthcare team can lead to successful outcomes.
What Can You Do?
If you have endometriosis and are concerned about your fertility, there are steps you can take to optimize your chances of conception:
- Adopt an anti-inflammatory diet: Eat foods rich in antioxidants, such as leafy greens, berries, turmeric, and omega-3 fatty acids, to combat oxidative stress and support egg quality.
- Consider medical treatment: Hormonal therapies like GnRH agonists, birth control pills, or progestin therapy may help manage symptoms and improve fertility outcomes.
- Support gut health: A balanced gut microbiome helps regulate inflammation. Incorporate probiotic-rich foods like yogurt, kefir, kimchi, and sauerkraut, or consider a high-quality probiotic supplement.
- Optimize lifestyle factors: Engage in regular, low-impact exercise like yoga or walking to reduce inflammation and support reproductive health. Prioritize stress management techniques, such as meditation or deep breathing, and ensure you’re getting enough quality sleep.
- Work with a fertility specialist: A reproductive endocrinologist or fertility dietitian can assess your specific needs and create a personalized plan, whether you’re trying to conceive naturally or exploring medical interventions.
- Discuss fertility preservation: If you’re not trying to conceive yet but may want to in the future, options like egg freezing can help safeguard your reproductive potential.
Final Thoughts
Endometriosis may make conception more challenging, but it doesn’t mean it’s out of reach. Every fertility journey is different, and while endometriosis can present obstacles, there are many ways to take control of your reproductive health. Whether through lifestyle changes, medical treatments, or working with a specialist, you have options. If you’re struggling, reach out to a healthcare provider to explore the best path for you. Knowledge is power, and by understanding the impact of this condition, you can approach your fertility journey with confidence and clarity.

Sources
https://pmc.ncbi.nlm.nih.gov/articles/PMC9983692
https://pmc.ncbi.nlm.nih.gov/articles/PMC8224039
https://www.rbmojournal.com/article/S1472-6483(13)00007-2/fulltext
https://pmc.ncbi.nlm.nih.gov/articles/PMC8065992
https://pmc.ncbi.nlm.nih.gov/articles/PMC7226034
https://pmc.ncbi.nlm.nih.gov/articles/PMC9528818
https://pmc.ncbi.nlm.nih.gov/articles/PMC10058497/#sec5-life-13-00654
https://pmc.ncbi.nlm.nih.gov/articles/PMC10820275

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Did you know that your gut health could impact more than just digestion? From immunity to mental clarity, a healthy gut plays a pivotal role in overall well-being—and even fertility. Emerging research suggests that a balanced gut microbiome influences hormone regulation, immune function, and inflammation, all of which are crucial for reproductive health. Whether you’re looking to optimize fertility or improve general health, supporting your gut can be a game-changer for both your body and mind.
The Basic Functions of the Gut
Before diving into the more intricate details of gut health, it’s essential to understand the basic functions of the gut and why it plays such a crucial role in your overall health.
1. Digestion
The gut is responsible for breaking down the food we eat, allowing nutrients to be absorbed into the bloodstream. This process starts in the mouth and continues through the stomach and small intestine. Enzymes and acids help break down food into smaller molecules for absorption.
2. Nutrient Absorption
Once food is broken down, the small intestine absorbs essential nutrients—like vitamins, minerals, and amino acids—into the bloodstream. These nutrients are then transported throughout the body to fuel our cells and organs.
3. Immune Function
A large portion of the body’s immune system resides in the gut. It acts as a barrier to harmful pathogens, such as bacteria and viruses. A healthy gut microbiome— the community of beneficial bacteria—supports immune function and helps protect the body from infections and inflammation.
4. Detoxification
The gut plays a vital role in detoxifying the body by processing and eliminating waste. The liver, bile, and gut work together to filter out toxins, which are then excreted through the stool. This process helps maintain a clean internal environment.
5. Hormone Regulation
The gut is involved in hormone production and regulation. It helps control hormones related to digestion, hunger, and metabolism. Additionally, the gut microbiome can influence hormonal balance, which is vital for reproductive health.
6. Gut-Brain Connection
The gut and brain communicate through the gut-brain axis, a direct link between the two. This connection influences mood, mental clarity, and stress levels. Research suggests that an imbalance in the gut microbiome can impact mental health conditions like anxiety and depression.
By understanding these basic functions, we can see why maintaining a healthy gut is essential for overall well-being and fertility. Now, let’s dive deeper into how to support these functions for optimal health.
Understanding Gut Permeability and Leaky Gut
Leaky gut occurs when the intestinal barrier becomes compromised, allowing undigested food particles, toxins, and microbes to enter the bloodstream. This process can trigger systemic inflammation and is implicated in conditions like autoimmune diseases, irritable bowel syndrome (IBS), and even neuroinflammation. The protein zonulin regulates tight junctions in the gut lining, and its overproduction is associated with increased gut permeability.
Dietary choices, stress, and environmental toxins all influence this delicate balance.
The Role of Diet in Gut Health
Diet plays a crucial role in shaping gut microbiota and maintaining a strong intestinal barrier. Research suggests that:
- High-fiber foods (e.g., fruits, vegetables, whole grains) support beneficial bacteria and help regulate gut permeability.
- Healthy fats, such as omega-3s, promote anti-inflammatory gut conditions, whereas excessive saturated fat intake can negatively impact gut flora.
- Akkermansia muciniphila, a beneficial bacterium, is linked to improved gut barrier function, reduced inflammation, and better metabolic health.
- Bovine colostrum supplementation has been shown to decrease intestinal permeability and lower zonulin levels, particularly in athletes.
Small Intestinal Bacterial Overgrowth (SIBO) and Gut Dysfunction
SIBO occurs when there’s an overgrowth of bacteria in the small intestine. This can lead to bloating, malabsorption, and digestive discomfort. It’s often associated with IBS, celiac disease, and metabolic syndrome.
Managing SIBO:
- Get proper testing to identify SIBO.
- Modify your diet, focusing on low FODMAP foods.
- Consider probiotics to restore balance.
- Work with a healthcare provider to determine if antibiotics are necessary.
Gut Health and Systemic Wellness
Emerging research highlights the gut-brain connection, linking gut health to cognitive function, mood regulation, and neurological diseases like Alzheimer’s. The gut microbiome also plays a role in cardiovascular health, obesity, and diabetes. Fecal microbiota transplants (FMT) have even been explored as potential treatments for age-related cognitive decline and metabolic disorders.
Gut Health and Fertility
Emerging research suggests that gut health plays a crucial role in reproductive health. The gut microbiome influences hormone regulation, immune function, and inflammation, all of which impact fertility outcomes. Dysbiosis, or an imbalance of gut bacteria, has been linked to conditions like polycystic ovary syndrome (PCOS), endometriosis, and unexplained infertility.
- Hormonal Balance: The gut microbiome helps regulate estrogen levels through the estrobolome, a collection of bacteria involved in estrogen metabolism. An imbalance can lead to estrogen dominance, which is associated with infertility and conditions like PCOS.
- Inflammation and Immune Function: Chronic inflammation, often driven by poor gut health, has been implicated in endometriosis and implantation failure. A healthy gut barrier helps regulate immune responses and supports a favorable reproductive environment.
- Microbiome and Pregnancy Outcomes: Research suggests that a balanced gut microbiome contributes to healthy pregnancy outcomes, reducing the risk of gestational diabetes, preeclampsia, and preterm birth.
Supporting Digestion
Efficient digestion breaks down food properly, allowing for optimal nutrient absorption and minimizing digestive distress.
Ways to enhance digestion include:
- Incorporating bitter foods: Foods like arugula, artichoke, bitter melon, dandelion greens, Brussels sprouts, coffee, and grapefruit stimulate stomach acid and bile production.
- Using digestive aids: Digestive enzymes, HCl supplements, apple cider vinegar, or digestive bitters may be beneficial.
- Relaxing at meals: Stress can negatively impact digestion, so mindful eating practices are essential.
- Consuming adequate minerals: Sodium (from sea salt) and zinc (from oysters and red meat) support stomach acid production.
Supporting Healthy Bile Flow
Bile is critical for fat digestion and detoxification. Signs of inadequate bile include bloating, floating stools, nausea after eating fats, and vitamin deficiencies. To support bile production:
- Consume fiber-rich foods: Legumes, beans, and avocados help bind to excess bile.
- Eat bitter foods: These naturally promote bile flow.
- Use cholagogue herbs: Globe artichoke, dandelion, burdock, and Oregon grape enhance bile movement.
- Ensure adequate taurine intake: Meat, fish, shellfish, and eggs aid in bile salt production.
Supporting Beneficial Bacteria
A balanced gut microbiome is essential for digestion, immunity, and gut barrier integrity. To nurture beneficial bacteria:
- Prioritize digestion first: Ensuring proper food breakdown is key before increasing fiber intake.
- Incorporate prebiotic foods: Apples, asparagus, garlic, onions, oats, and legumes serve as fuel for gut bacteria.
- Limit excessive alcohol intake: Alcohol can cause dysbiosis and inflammation.
Supporting Liver Detoxification
The liver plays a crucial role in gut health through bile production and detox processes. To support liver function:
- Include Phase 1 detox foods: Magnesium (leafy greens, avocado), B vitamins (liver, eggs, seafood), vitamin C (citrus, bell peppers), and zinc (oysters, beef).
- Incorporate Phase 2 detox foods: Glycine (bone broth), glutamine (beef, spinach), cysteine (broccoli, eggs), and taurine (meat, fish).
Strengthening the Gut Lining
A strong intestinal barrier prevents harmful substances from entering the bloodstream. Factors that contribute to a leaky gut include stress, poor digestion, processed foods, overuse of medications, and imbalanced gut bacteria. To support gut integrity:
- Limit inflammatory foods: Avoid heavily processed and inflammatory oils.
- Boost beneficial fibers: Prebiotic and resistant starch-rich foods enhance gut lining health.
- Consume gut-supportive nutrients: Glutamine (cabbage, fish), zinc (beef, crab), and colostrum aid in healing the gut lining.
- Use gut-healing herbs: Marshmallow root, slippery elm, aloe vera, and licorice can be beneficial.
Strengthening the Immune System
A well-functioning immune system relies on strong digestion and a balanced gut microbiome. Factors that deplete immunity include poor digestion, chronic stress, hormonal imbalances, and long-term medication use. To support immune health:
- Improve digestion and gut microbiome health
- Incorporate immune-boosting foods: Colostrum, mushrooms (reishi, shiitake), and vitamin C-rich foods (citrus, mango, papaya) support immune function.
- Use supportive herbs: Andrographis, elderberry, echinacea, and astragalus help strengthen immunity.
Prebiotics & Resistant Starch
Prebiotics are fibers that feed beneficial bacteria and help produce short-chain fatty acids, which support gut integrity and immunity.
- Prebiotic foods: Apples, asparagus, garlic, onions, oats, and legumes.
- Resistant starch sources: Cooked and cooled potatoes, green bananas, and legumes.
By focusing on these key areas, you can create a solid foundation for optimal gut health and overall well-being. Making small, sustainable changes to your diet and lifestyle can have lasting positive effects on digestion, immunity, and energy levels.
Conclusion
Maintaining gut health is essential for overall well-being, from digestion and immunity to mental clarity and chronic disease prevention. By making mindful dietary and lifestyle choices, you can support a resilient gut microbiome and improve long-term health outcomes. The science is clear: a healthy gut is a foundation for a thriving body and mind.

Sources
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6996528/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8305009/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6313445/
- https://pubmed.ncbi.nlm.nih.gov/38790992/
- https://pubmed.ncbi.nlm.nih.gov/32023228/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8058106/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8674859/
- https://pubmed.ncbi.nlm.nih.gov/25290618/
- https://pubmed.ncbi.nlm.nih.gov/35874661/
- https://pubmed.ncbi.nlm.nih.gov/34623232/
- https://www.imrpress.com/journal/FBL/26/5/10.52586/4921/htm
- https://www.nia.nih.gov/news/beyond-brain-gut-microbiome-and-alzheimers-disease
- https://pubmed.ncbi.nlm.nih.gov/34054740/
- https://pubmed.ncbi.nlm.nih.gov/28397754/
- https://pubmed.ncbi.nlm.nih.gov/35745242/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7971312/
- https://pubmed.ncbi.nlm.nih.gov/28778332/

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Cervical health is a vital aspect of women’s overall well-being, encompassing the maintenance of the cervix—the lower, narrow part of the uterus that connects to the vagina. A healthy cervix plays a crucial role in reproductive health, acting as a barrier to infections and facilitating childbirth. While regular medical screenings and vaccinations are essential components of cervical care, adopting natural approaches can further support and enhance cervical health. This article delves into various natural strategies, including nutrition, lifestyle modifications, and herbal remedies, to promote optimal cervical well-being.
Understanding the Cervix
The cervix is a critical structure within the female reproductive system, serving multiple functions that support fertility, pregnancy, and overall gynecological health. It is approximately 2 to 3 centimeters long and is composed of dense connective tissue and smooth muscle. The cervix connects the uterus to the vagina and has a small opening, known as the cervical os, which changes throughout a woman’s life and menstrual cycle.
One of the cervix’s primary functions is to regulate the passage of substances between the uterus and the vagina. The cervical mucus produced by specialized glands within the cervix plays a key role in this process. During ovulation, the mucus becomes thinner and more slippery, facilitating sperm movement toward the egg. In contrast, outside the fertile window, cervical mucus thickens to form a protective barrier that helps prevent infections from ascending into the uterus.
During pregnancy, the cervix undergoes significant changes to support fetal development. It remains firm and closed to keep the developing baby secure in the uterus. In the final weeks of pregnancy, the cervix gradually softens, shortens, and dilates in preparation for labor. This process, known as cervical effacement and dilation, is essential for a smooth delivery.
The cervix also plays a crucial role in protecting against infections. It serves as a physical barrier, preventing harmful bacteria and viruses from entering the uterus. The cervix’s immune response, including the production of antimicrobial proteins and immune cells, helps maintain a balanced vaginal microbiome. An imbalance in the cervical and vaginal microbiota can increase susceptibility to infections such as bacterial vaginosis and sexually transmitted infections (STIs), including human papillomavirus (HPV), which is a major risk factor for cervical cancer.
Cervical health has influence on various factors, including hormonal changes, immune function, and lifestyle choices. Regular Pap smears and HPV tests are essential for detecting early changes in cervical cells that could indicate precancerous conditions. Additionally, maintaining a nutrient-rich diet, avoiding tobacco use, and practicing safe sex can significantly contribute to cervical well-being.
The Role of Nutrition in Cervical Health
A balanced diet rich in specific nutrients can significantly impact cervical health by supporting the immune system, promoting healthy cell function, and reducing the risk of infections and diseases. Research indicates that certain vitamins and minerals are particularly beneficial:
- Vitamin C: Known for its immune-boosting properties, vitamin C enhances collagen production, which maintains cervical tissue integrity. It also acts as an antioxidant, reducing oxidative stress that contributes to cervical abnormalities. Incorporate citrus fruits, bell peppers, strawberries, and broccoli into your diet.
- Beta-Carotene & Vitamin A: These nutrients are essential for epithelial cell health, which includes cervical cells. Vitamin A supports immune function and promotes cell differentiation, reducing the risk of dysplasia. Sources include carrots, sweet potatoes, spinach, and kale.
- Folate (Vitamin B9): Folate plays a critical role in DNA synthesis and repair, reducing the likelihood of abnormal cervical cells. A diet rich in leafy greens, legumes, avocados, and citrus fruits ensures adequate intake.
- Vitamin E: This powerful antioxidant protects cervical cells from oxidative stress and supports reproductive health. Nuts, seeds, spinach, and sunflower oil are excellent sources.
- Zinc: Zinc supports immune function, aids in DNA repair, and promotes healthy cell division. It is found in meats, dairy, nuts, and whole grains.
- Probiotics: A healthy cervical and vaginal microbiome is crucial in preventing infections and maintaining pH balance. Fermented foods such as yogurt, kimchi, and sauerkraut help introduce beneficial bacteria that support immune function.
- Omega-3 Fatty Acids: These essential fats have anti-inflammatory properties that help regulate immune responses and support cell integrity. Sources include fatty fish, flaxseeds, and walnuts.
Incorporating these nutrients into your diet can be achieved by consuming a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats. For instance, a salad with spinach, kale, shredded carrots, and sunflower seeds, accompanied by a citrus-based dressing, can provide a nutrient-dense meal supportive of cervical health.
Foods and Substances to Limit or Avoid
While certain foods can enhance cervical health, others may have detrimental effects and should be consumed in moderation:
- Processed Foods: High levels of preservatives and additives in processed foods can contribute to inflammation and negatively impact overall health.
- Sugary Beverages: Excessive sugar intake is linked to inflammation and an increased risk of infections. Opt for water, herbal teas, or natural fruit juices instead.
- High-Fat Dairy Products: Saturated fats found in high-fat dairy products may negatively affect cellular health and immune function. Choosing low-fat or plant-based dairy alternatives can be beneficial.
- Processed Meats: Diets high in processed meats are found to be associated with increased inflammation and a higher risk of certain cancers. Incorporating plant-based proteins or lean meats can be a healthier alternative.
- Alcohol: Excessive alcohol consumption is linked to an increased risk of cervical cancer and can compromise the immune system. Limiting alcohol intake can help maintain cervical health.
Lifestyle Modifications for Cervical Health
Beyond diet, lifestyle habits play a crucial role in maintaining cervical well-being. Small changes can make a big difference in overall health.
Regular Physical Activity
Engaging in regular exercise helps maintain a healthy weight, reduces stress, and strengthens the immune system. Activities like walking, yoga, or strength training can improve circulation and overall reproductive health.
Avoiding Tobacco Use
Smoking is a significant risk factor for cervical cancer. It weakens the immune system, making it harder for the body to fight off HPV infections. Quitting smoking can dramatically reduce this risk and improve overall well-being.
Practicing Safe Sex
Using condoms and limiting the number of sexual partners can lower the risk of HPV and other STIs. Since HPV is a leading cause of cervical cancer, safe sex practices are vital for prevention.
Managing Stress
Chronic stress weakens the immune system, making the body more susceptible to infections. Stress management techniques such as meditation, yoga, deep breathing exercises, or spending time in nature can promote overall health, including cervical wellness.
Herbal Remedies and Supplements
Traditional practice incorporates herbs and supplements to support cervical health:
- Green Tea: Green tea contains polyphenols, which are antioxidants known for their potential cancer-fighting properties. Regular consumption of green tea may contribute to cervical health by combating oxidative stress and inflammation.
- Turmeric: Curcumin, the active compound in turmeric, has anti-inflammatory and antioxidant properties. Adding turmeric to your diet may help maintain cervical health by reducing inflammation and supporting the body’s defense mechanisms.
- Turkey Tail Mushroom: Turkey tail mushrooms (Coriolus versicolor) are used in traditional Chinese medicine for their immune-boosting properties. They contain polysaccharide K (PSK) and polysaccharopeptide (PSP), which enhance immune health and may help fight HPV infections.
Integrating Functional Nutrition into Daily Life
A practical way to incorporate these nutrients into your daily routine is by creating meals that support cervical health. For instance:
- A smoothie made with spinach, kale, banana, Greek yogurt, and flaxseeds provides essential vitamins, probiotics, and omega-3s.
- A salad with mixed greens, shredded carrots, sunflower seeds, and grilled salmon delivers a nutrient-dense meal that promotes cervical integrity.
- Herbal teas with green tea and turmeric can offer daily antioxidant and anti-inflammatory benefits.
In Closing
Cervical health is a vital component of overall well-being, and taking proactive steps to support it naturally can be highly beneficial. By incorporating a nutrient-rich diet, adopting healthy lifestyle habits, and considering natural remedies, individuals can promote cervical health and reduce the risk of complications. Regular medical check-ups, including Pap smears and HPV testing, remain essential for early detection and prevention. A holistic approach that combines medical care with natural strategies can empower individuals to maintain optimal cervical health throughout their lives.

Sources:
https://pmc.ncbi.nlm.nih.gov/articles/PMC7698010
https://pmc.ncbi.nlm.nih.gov/articles/PMC4997408

Written by: Lauren Chamberlain
Edited and Reviewed By: Anabelle Clebaner MS, RDN
Thinking about starting a family? Have you ever wondered what you can do before trying to conceive to boost your chances of a healthy pregnancy? Your fertility journey starts long before a positive pregnancy test. Preparing for pregnancy isn’t just about tracking ovulation and taking prenatal vitamins—it’s about optimizing your entire body for conception and a healthy pregnancy. Scientific research increasingly shows that preconception health plays a crucial role in reproductive success and fetal development. Here are five key areas you can’t afford to skip when getting ready to grow your family.
1. Support Your Gut Health
Your digestive system isn’t just about breaking down food—it’s a complex ecosystem that plays a central role in your overall health, including fertility. A healthy gut microbiome, which refers to the trillions of bacteria, fungi, and other microbes living in your digestive system, influences numerous physiological functions, from hormone regulation to immune function and even mood.
The connection between gut health and fertility is emerging as an important area of study. Research increasingly shows that an imbalanced gut microbiome, also known as dysbiosis, can have a significant impact on fertility. When the gut microbiome is out of balance, it can lead to inflammation, hormonal imbalances, and poor nutrient absorption—all of which can affect your ability to conceive.
The Gut Microbiome and Hormone Regulation
A healthy gut microbiome is essential for maintaining hormonal balance, which is crucial for fertility. The gut bacteria help metabolize estrogens, which are important for regulating the menstrual cycle and maintaining a healthy ovulation pattern. Dysbiosis has been linked to estrogen dominance, which can interfere with ovulation and lead to conditions like polycystic ovary syndrome (PCOS), a common cause of infertility.
The microbiome also plays a key role in detoxifying estrogen and other hormones, helping to prevent an overload of hormones that can disrupt your reproductive system. When the gut is not functioning optimally, it can lead to a build-up of excess estrogen in the body, a condition known as estrogen dominance, which can impact fertility and cause other reproductive health problems.
Gut Health and Immune Function
In addition to influencing hormones, the gut microbiome also affects your immune system. Around 70% of the body’s immune cells reside in the gut, and the microbiome plays a vital role in maintaining immune balance. A healthy immune system is essential for fertility because an overactive or dysfunctional immune response can interfere with embryo implantation and fetal development. Chronic inflammation in the gut can trigger an autoimmune response, leading to complications in fertility and pregnancy.
Studies have shown that women with autoimmune diseases, such as endometriosis or thyroid disorders, often have gut dysbiosis, which could be contributing to their fertility struggles. This means addressing gut health may also help reduce inflammation and autoimmune responses, creating a more favorable environment for conception and pregnancy.
The Role of Diet in Gut Health
Your diet plays a crucial role in shaping your gut microbiome. The foods you eat provide fuel for your gut bacteria, and by choosing nutrient-dense, whole foods, you can encourage the growth of beneficial microbes that support both gut and reproductive health.
To promote a healthy gut microbiome and support fertility:
- Eat fiber-rich foods: A diet high in fruits, vegetables, whole grains, and legumes provides the necessary fiber to feed beneficial gut bacteria. Fiber acts as a prebiotic, helping to nourish the good bacteria in your gut that help regulate hormones and immune function.
- Include fermented foods: Fermented foods such as yogurt, kefir, sauerkraut, kimchi, and kombucha contain probiotics, which are live beneficial bacteria that help restore balance to the gut microbiome. These foods support the growth of healthy bacteria, improve digestion, and reduce inflammation, all of which are essential for fertility.
- Limit processed foods and sugar: Processed foods, refined sugars, and artificial sweeteners can encourage the growth of harmful bacteria in the gut, leading to an imbalance in the microbiome. This imbalance can contribute to inflammation and poor immune function, both of which can hinder fertility.
Addressing Gut Dysbiosis for Fertility
If you suspect that gut dysbiosis may be affecting your fertility, it’s important to work with a healthcare professional, such as a dietitian or functional medicine practitioner, to assess and address the issue. Common signs of dysbiosis include digestive symptoms like bloating, gas, constipation, diarrhea, and food intolerances. A professional can help guide you through dietary changes and supplements, such as probiotics or antimicrobial herbs, to support gut health and restore balance to your microbiome. Some studies have suggested that the use of probiotics and other gut-healing supplements may improve fertility outcomes, particularly in women with PCOS and other reproductive health conditions.
By supporting your gut health, you’re not just promoting better digestion and immune function—you’re creating a favorable environment for fertility.
Learn more about gut health and fertility
2. Balance Blood Sugar
Maintaining balanced blood sugar is crucial for overall health, especially when preparing for pregnancy. Blood sugar imbalances, such as insulin resistance and high blood glucose levels, can interfere with ovulation, hormone production, and overall fertility. In fact, managing blood sugar levels can be one of the most effective ways to optimize reproductive health and enhance fertility. Here’s why blood sugar balance matters and how you can achieve it.
How Blood Sugar Affects Fertility
Blood sugar imbalances, particularly insulin resistance, can have a significant impact on fertility. Insulin is a hormone that regulates blood sugar levels, and when the body becomes resistant to insulin, it needs to produce more of it to maintain normal blood glucose levels. High insulin levels can disrupt the balance of other hormones that regulate reproductive function, such as estrogen, progesterone, and testosterone. In addition to disrupting ovulation, high insulin levels can also impact the quality of the eggs and the ability to support a pregnancy.
The Link Between Blood Sugar and Hormone Imbalance
The relationship between blood sugar and hormone balance is intricate. Insulin not only regulates glucose levels but also interacts with other hormones like cortisol, leptin, and thyroid hormones, all of which play essential roles in fertility. High insulin levels can lead to an imbalance in these hormones, affecting reproductive function.
For example:
- Cortisol: Chronic stress and high blood sugar levels can elevate cortisol, a stress hormone that disrupts hormone production and reduces fertility. High cortisol levels can lead to irregular menstrual cycles and impair ovulation.
- Leptin: Leptin is a hormone produced by fat cells that helps regulate appetite, metabolism, and reproductive function. Imbalances in leptin levels, often seen in individuals with insulin resistance, can interfere with ovulation and menstrual regularity.
- Insulin resistance can also disrupt thyroid function, which is crucial for fertility. Studies have shown that insulin resistance can lead to hypothyroidism (low thyroid function), which can cause menstrual irregularities, poor egg quality, and difficulty getting pregnant.
How to Balance Blood Sugar for Fertility
Achieving and maintaining stable blood sugar levels is a key factor in preparing for pregnancy. Here are some practical steps you can take to balance your blood sugar:
Prioritize Protein, Fiber, and Healthy Fats
Including a balance of protein, fiber, and healthy fats at each meal can help stabilize blood sugar levels. These nutrients slow the absorption of glucose into the bloodstream, preventing spikes in blood sugar. Focus on lean protein sources (such as chicken, fish, tofu, and legumes), fiber-rich vegetables and whole grains, and healthy fats (like avocado, nuts, and olive oil).
Minimize Refined Carbs and Sugar
Refined carbohydrates (such as white bread, pasta, and baked goods) and sugary foods cause rapid spikes in blood sugar, followed by crashes that can lead to insulin resistance over time. Instead, opt for whole grains, vegetables, and fruits that release sugar more slowly into the bloodstream, providing a steady supply of energy.
Regular Physical Activity
Exercise, especially strength training, helps improve insulin sensitivity, meaning your body uses insulin more effectively to regulate blood sugar. Studies have shown that regular physical activity, including moderate aerobic exercise and strength training, can improve metabolic function and support healthy hormone levels, thereby enhancing fertility.
Manage Stress
Chronic stress can elevate cortisol levels, which in turn disrupt blood sugar regulation and fertility. Incorporating stress-management techniques such as deep breathing, meditation, yoga, or spending time in nature can help lower cortisol levels and improve overall hormonal balance.
Consider Supplements
Certain nutrients, such as magnesium, chromium, and omega-3 fatty acids, may help support healthy blood sugar metabolism. Magnesium, in particular, is important for insulin function, and research has shown that adequate magnesium levels are associated with better fertility outcomes.
Managing blood sugar not only supports fertility but also helps set the stage for a healthy pregnancy by lowering the risk of complications like gestational diabetes.
Explore blood sugar management strategies
3. Detox Your Environment
Endocrine-disrupting chemicals (EDCs), found in plastics, pesticides, pollution, and personal care products, can interfere with hormone balance and reproduction. Research shows that exposure to EDCs—such as BPA, phthalates, and pesticides—can affect fertility by disrupting hormone production and ovarian function.
The 4 P’s to Avoid:
- Plastics: Opt for glass or stainless steel for food storage and drink containers to reduce exposure to BPA and phthalates, which have been linked to reduced ovarian reserve and lower sperm quality.
- Pesticides: Choose organic produce when possible and thoroughly wash fruits and vegetables. Pesticides can disrupt estrogen and progesterone levels, hindering reproductive success.
- Pollution: Use air purifiers and avoid high-traffic areas to minimize exposure to air pollution, which can lower fertility rates and increase miscarriage risk.
- Personal Care Products: Swap conventional beauty, skincare, and cleaning products for non-toxic alternatives. Parabens and synthetic fragrances found in many products are linked to hormone disruption and reduced fertility.
Reducing your exposure to these toxins can help protect your hormones and reproductive health.
Learn more about reducing toxic exposure
4. Optimize Sleep & Manage Stress
Poor sleep and chronic stress can raise cortisol levels, negatively impacting reproductive hormones and fertility. Disrupted sleep patterns—such as waking up between 1-3 AM—may indicate liver detoxification issues, while difficulty staying asleep or waking up feeling unrested often correlates with low progesterone levels. Stress can lead to irregular cycles, making conception more difficult.
Studies show that sleep disturbances and high stress levels can disrupt menstrual cycle regularity, reduce ovarian function, and even affect early pregnancy outcomes.
To improve sleep and reduce stress:
- Stick to a consistent sleep schedule, even on weekends.
- Avoid blue light exposure from screens at least an hour before bed.
- Create a calming nighttime routine—try magnesium, herbal teas, or journaling.
- Get sunlight exposure in the morning to regulate circadian rhythms.
Stress-reducing activities like meditation, breathwork, and yoga can support your fertility by lowering cortisol levels.
5. Assess Your Partner’s Health
Fertility is a team effort! Around 40% of infertility cases involve male factors, and sperm health plays a major role in conception. Changes in diet, lifestyle, and environmental exposure can improve sperm quality, motility, and count. Since sperm takes about 74 days to regenerate, it starts by making changes at least three months before conception.
To support male fertility:
- Nutrient-dense foods rich in zinc, selenium, omega-3 fatty acids, and antioxidants are essential for sperm health. Zinc and selenium, in particular, play critical roles in sperm formation and motility.
- Limit alcohol and cannabis use, as both can reduce sperm concentration and motility.
- Avoid excessive heat—hot tubs, saunas, and even laptops on laps can lower sperm count. The testes require a cooler temperature for optimal sperm production.
- Reduce stress—high cortisol levels can lower testosterone and sperm quality.
The father’s lifestyle before conception can influence the baby’s long-term health through epigenetic changes, which may affect gene expression in both parents.
Learn more about understanding cortisol
The Bottom Line
Prepping for pregnancy isn’t just about waiting for a positive test—it’s about creating the healthiest possible environment for conception and beyond. By addressing gut health, blood sugar balance, environmental toxins, sleep, and both partners’ health, you’re laying the groundwork for a smoother fertility journey. Small, intentional choices today can make a big difference tomorrow. Take control of your health today!
Start your journey to optimal fertility

Sources
https://pmc.ncbi.nlm.nih.gov/articles/PMC9603966
https://pmc.ncbi.nlm.nih.gov/articles/PMC5052775
https://www.sciencedirect.com/science/article/pii/S245196502030079X
https://www.cdc.gov/genomics-and-health/epigenetics/index.html
https://www.hopkinsmedicine.org/health/wellness-and-prevention/planning-a-pregnancy
https://pmc.ncbi.nlm.nih.gov/articles/PMC6075697
https://pmc.ncbi.nlm.nih.gov/articles/PMC4145858

The Preconception Playbook
This free playbook provides specific actionable tips to get started on your fertility journey, as well as what to avoid while you're trying to conceive.
Get the free playbook